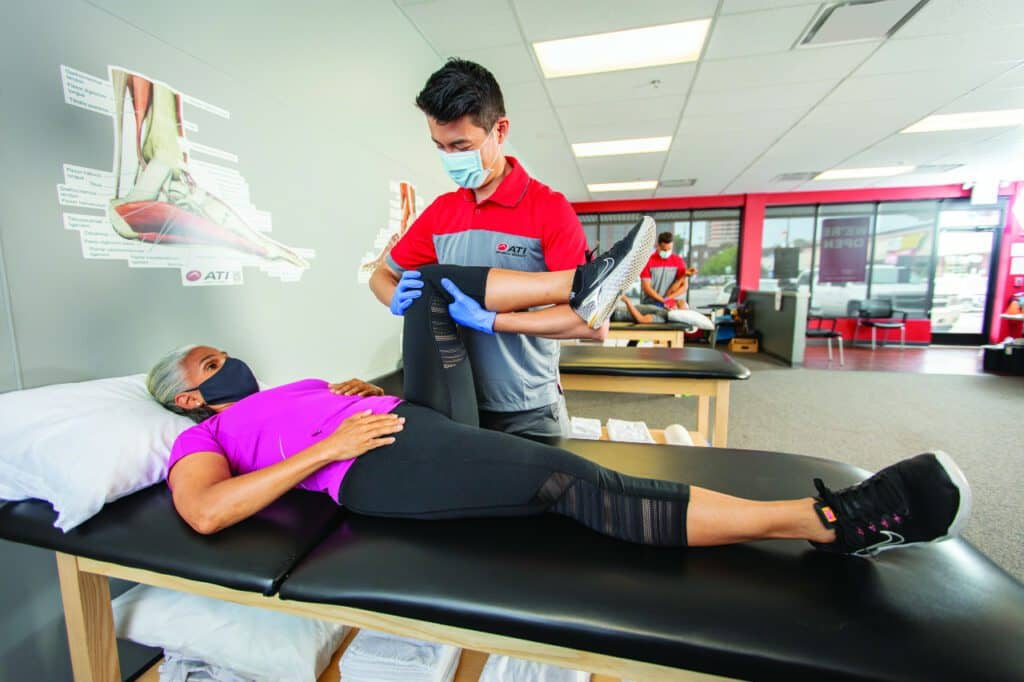
PHOTO CAPTION: Telehealth PT treatment can provide long-term relief and improvement of function in patients with various conditions.
As more clinics begin opening their doors to patients after relying on remote options, it’s worth considering whether one is better than the other.
By Therese Casey, PT, DPT, and Gerald Dolce, PT, DPT, Cert-DRN, COMT, OCS
Telehealth’s Impact on Healthcare and Physical Therapy
Telemedicine, aka telehealth, has been rapidly growing over the past 5 years. Due to the COVID-19 pandemic, we have seen even more of an increase in demand for this service. While the pandemic is starting to slow, telehealth should remain an option for patients, as it accommodates travel and busy schedules. Rapidly evolving telemedicine has been able to provide increased access to high-quality healthcare and is cost-effective.
Further Reading: Overcoming Telehealth Barriers for Stroke Survivors
According to the Centers for Medicare and Medicaid Services (CMS), telemedicine is “a service that seeks to improve a patient’s health by permitting two-way, real-time interactive communication between the patient and the physician at a distant site.”¹ The concern in the physical therapy field remains: Which is better, telemedicine or in-clinic care? In order to answer this question, we have to dive into different diagnoses as well as visit how it may impact the care performed at home and in the clinic.
[sidebar float=”right” width=”250″]Product Resources
The following companies provide equipment that can be used for treatment in the home:
Dynatronics
https://www.dynatronics.com
Exertools
https://exertools.com
Magister
https://magistercorp.com
MediCordz by NZ Manufacturing Inc
https://nzcordz.com/medicordz/
NZ Manufacturing Inc
https://nzcordz.com
Pro-Tec Athletics
https://www.pro-tecathletics.com
Stretchwell Inc
https://www.stretchwell.com[/sidebar]
Benefits of In-Person Treatment
For certain conditions, in-person treatment has invaluable effects. The three major benefits of in-person treatment include manual therapy techniques, patient education, and ensuring proper body mechanics.
Manual Therapy
Manual therapy can consist of joint mobilizations, soft tissue mobilization, massage, scar mobilization, trigger point dry needling, Graston Technique, cupping, and more. These techniques require the skills of a licensed healthcare professional to be effective and safely completed. This is arguably the most skilled part of physical therapy and can make a significant impact on a patient’s pain management and recovery.
For example, a patient may require ankle joint mobilizations to improve motion needed to go down stairs. An individual with chronic headaches would likely benefit from a suboccipital release or dry needling to cervical muscles. Or a PT completing the Epley’s maneuver can fully resolve problems with dizziness for a patient who suffers from vertigo. These are techniques only a professional can perform and, ultimately, the power of touch helps to build rapport and trust with a patient.
Patient Education
For patients to fully understand their condition and appreciate the relevance of their treatment, education is key. Whether using a spine model, Netter Anatomy book, or layman’s terms, it is a PT’s role to convey the source of the condition and provide guidance on how to effectively manage it. For instance, a patient may not understand how pain in their back is causing numbness or tingling down their leg, or why weakness in their hips is causing pain on their outer knee.
After explaining how these items are interconnected, it is also necessary to ensure the patient understands why they are doing the therapeutic exercises that have been advised. For example, a PT can explain that they are performing sciatic nerve glides to decrease neural tension and subsequent tingling, or performing glute strengthening to prevent hip drop and subsequent knee pain while jogging.
Education can also be provided on self-mobilization techniques and utilization of therapy equipment to promote carryover between sessions and maintenance of therapeutic gains upon discharge. Patient education should start on day one and continue through the entirety of the plan of care.
Body Mechanics
Proper body mechanics are crucial to reduce stress on affected body regions and prevent reinjury. Squat form, gait mechanics on treadmill, and overhead lifts without compensation are examples of functional activities that require a skilled eye. Various views of squat, slow-motion video assessment on treadmill, and tactile cues to reduce excess upper trap activation during lifting help to ensure safe completion of these activities. Demonstration and feedback by a PT allow for improved comprehension of form by a patient.
While it could be argued that aspects of in-person treatment could be accomplished via telehealth, it would not be to the same degree. Personal touch and human interaction act as major drivers to patient success.
In Clinic vs At Home
As we look to expand how telehealth can contribute as a player in the future of healthcare, there are certain diagnoses that may be more advantageous to treat at home versus in the clinic. For example, much of low back research suggests that helping patients participate in functional movement helps improve symptoms over a set period of time, which could be completed at home. On the other hand, postoperative total hip arthroplasty (THA) may be better suited for in-clinic treatment. In the clinic, not only can a physical therapist provide guidance for maintaining hip precautions, but the postoperative THA patient also has access to the manual techniques the PT can perform and to certain equipment that may not be as readily available at home.
Further Reading: Revised Guidelines Regarding Cognitive Rehabilitation After TBI Focus on Telehealth
Whether in the clinic or at home, telehealth physical therapy clearly provides benefits and positive outcomes. It may be able to provide long-term relief and improvement of function for patients with various conditions. For example, in a trial of patients managed with total knee arthroplasty (TKA), a virtual PT program with skilled telerehabilitation was determined to be as effective as traditional PT for addressing function and disability and as safe as traditional PT in terms of pain and rehospitalization.² These findings suggest that virtual PT with a telehealth therapist for remote clinical monitoring and guidance should be considered for patients after TKA.² Overall, early intervention, consistency in treatment, and patient engagement will set up a patient for a successful outcome, regardless of the setting.
Equipment for In-Clinic and At Home
At-home equipment can have multiple advantages. First off, a patient can achieve similar results after successfully going through a demonstration in the clinic.
Traction
For example, a patient who is suffering from either cervical or lumbar discogenic pain may be able to obtain home lumbar and cervical traction units. In the clinic, we can utilize equipment such as the Chattanooga TX traction unit from Chattanooga Medical Supply, Chattanooga, Tenn, which can help with decompression, guided by the recommended parameters from the therapist. Fortunately, we can also achieve these same results with units such as ComforTrac CT by Zynex Medical, Englewood, Colo, which is more affordable and available for purchase by the patient. These units may also be covered by insurance, which makes them a more feasible option to continue treatment virtually once proper direction is given by the licensed clinician.
Strength and Conditioning
There are other conditions for which strength and conditioning equipment would be more appropriate. ACL reconstruction, ankle sprains, femoral acetabular impingement, and shoulder impingement are just a handful of conditions that would benefit from a structured program of progressive loading. An example would be increasing strength production after ACL reconstruction. After the initial stages of mini squat, progressing into 90-90 squatting at home with utilization of resistance bands can help make these exercises more challenging for the individual. Specifically, Cando Resistance bands made by Chattanooga Medical Supply can provide resistance to the lower extremities by stepping on the bands, creating a downward resistance effectively working lower extremity musculature.
Large
In-clinic equipment can be expensive and large, making it difficult to have at home. Something such as a simple leg press machine would not only suffice in strength production, but also to help improve knee range of motion for those progressing through ACL reconstruction, THA, and TKA. Having this type of equipment at the clinic is a benefit of attending in-person therapy sessions. The Cybex VR3 Leg Press made by Cybex International, Medway, Mass, is an example of a safe and effective machine that can achieve this in the clinic.
Small
We can also look to smaller equipment that can achieve balance and proprioception goals with this same patient population. The Fitterfirst Rockerboard from Fitterfirst in Calgary, Alberta, Canada, is a piece of equipment that we use in the clinic for this purpose. This is known as a professional device and would not be available to the general population.
Balance is a key ingredient in the treatment plan of patients with various conditions. Specifically, for patients who have a postoperative status, it may be beneficial for them to have a therapist to guard movements when using the Rockerboard as this may be unsafe for a patient to independently perform within their home, even if they did have access to one there. But the lack of availability of certain necessary equipment in patients’ homes is another example of how in-clinic treatment can provide benefits over telehealth.
Transitioning
As we look to achieve the best possible outcomes for our patients, we can select the best pieces of equipment to enhance recovery and advance patients in their treatment program. Once we achieve desired goals utilizing manual therapy, in-clinic equipment with therapist direction, and patient education, we can direct the patient to start to perform similar activities at home. Allowing patients to become independent and assisting them to acquire pieces of equipment that promote established goals set on the initial evaluation date will promote self-efficacy.
A Matter of Choice
To answer the question, “Is telehealth or in-clinic physical therapy superior?” we argue that both have an appropriate place in the healthcare field, but it ultimately depends on a patient’s condition and their access to technology as well as therapeutic equipment. A patient should select whichever treatment method allows them to feel most comfortable while at the same time maximizes their outcomes. PTP
Therese Casey, PT, DPT, is a physical therapist and clinic director at ATI Physical Therapy in Chicago. She received her Doctorate in Physical Therapy from Marquette University in 2017 and has been practicing as a PT at ATI for 4 years.
Gerald Dolce, PT, DPT, Cert-DRN, COMT, OCS, is a physical therapist and clinic director at ATI Physical Therapy in Las Vegas, specializing in advanced orthopedic conditions. A graduate from the Touro University Nevada physical therapy program, Dolce has been a practicing PT since 2017. For more information, contact [email protected].
References
- Kichloo A, Albosta M, Dettloff K, et al. Telemedicine, the current COVID-19 pandemic and the future: a narrative review and perspectives moving forward in the USA. Fam Med Community Health. 2020;8(3):e000530 doi: 10.1136/fmch-2020-000530
- Prvu Bettger J, Green CL, Holmes DN, et al. Effects of virtual exercise rehabilitation in-home therapy compare with traditional care after total knee arthroplasty. J Bone Joint Surg. 2020;102(2):101-109.





