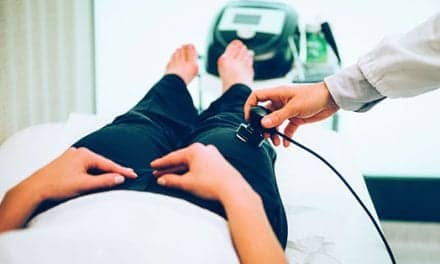
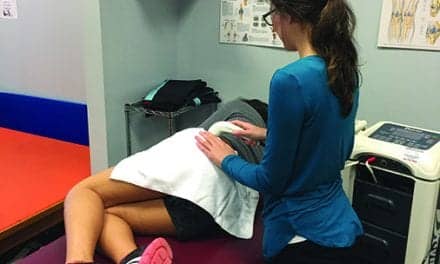
Topical analgesics, including those with CBD, are effective as a complement to other pain management strategies in physical therapy practice.
By Erson Religioso III, DPT, MS, MTC, CFC, CertMDT, CertMST, CNPT, FAAOMPT
Pain management represents a significant unmet need generally, but especially in circumstances where patients require physical rehabilitation. Topical pain treatments, including both prescription and over-the-counter products, are safe and effective options for certain pain conditions when systemic administration is either undesirable or unnecessary. Topical agents include creams, ointments, patches, and gels based on either reformulated oral drugs, or non-pharmaceutical active ingredients. Let’s take a look at one such agent in particular: cannabidiol, or CBD.
A strong case may be made for further investigating cannabidiol based on three factors: clinical and preclinical evidence, the molecule’s myriad interactions with around 80 human receptors and pathways associated with pain, and established strategies for topical dosage form development.
Main Photo Caption: Physical therapist Erson Religioso III regularly uses topical analgesics, including those containing CBD, to help manage his clients’ pain. Photo: Erson Religioso III
Complementary Treatment
Individuals enter physical rehabilitation programs for conditions arising from injury, medical procedures, the consequences of lifestyle choices, the effects of normal aging, or some combination of “all of the above.” Many of these conditions involve the need for the relief of chronic or acute pain.1
Related: Pain Management Product Showcase
Rehabilitation utilizes a range of treatments including exercise to help improve strength, range of motion, function, and quality of life. Many rehab clients also benefit from physical or mechanical modalities such as ultrasound2, electrical stimulation3 including TENS (transcutaneous electrical neuromuscular stimulation4), joint mobilization5, heat or cold6, and whirlpool therapy7 to manage pain. In addition, manual therapy including joint and soft tissue manipulation, which loosen and address injured tissues, may be used in combination with other modalities to decrease pain, improve circulation, and decrease muscle tension.8 All of these can often be complemented by topical pain agents.
Topical Agents in the Clinic
Many treatments utilized in a physical rehabilitation setting, particularly those targeting mild to moderate pain, may be enhanced through application of topical pain agents including salicylates, anesthetics, capsaicin, alpha adrenoreceptor agonists, nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, and cannabinoids.9
Although topical medications are somewhat limited to treating mild-to-moderate pain originating on or near the surface of the skin, these treatments provide several benefits, some of them unique to topical application.
Topical agents are effective against both acute pain (sprains, tendonitis, acute back pain, muscle aches) and the pain associated with chronic conditions such as osteoarthritis, chronic lower back pain, and some neuropathies.10
Since the active ingredients in almost all topically applied drugs are small molecules (vs. biologics), they may be blended with a wide range of excipients, emulsifiers, and other active or inactive ingredients into almost any suitable dosage form, including creams, ointments, patches, etc. Formulations are stable over a wide range of temperatures, and may be selected for pharmacokinetics as well, for example with rapid or slow release/delivery. 11
PRODUCT RESOURCE: Topical Analgesics
These companies offer topical analgesics that can be used for pain management:
Elrt Technologies
Parker Laboratories
Sore No More
Working Locally
Although some topical pain drugs (e.g. opioids) undergo systemic distribution, most products penetrate and work locally, at the skin or into tissue right below the surface.12 This is both a benefit and a drawback: Low systemic uptake limits the scope of pain treatable topically, but it also greatly reduces or eliminates systemic side effects.
For example, many NSAIDs, originally introduced as oral or injectable systemically distributed drugs, have been reformulated for topical administration. Several topical versions of these drugs—including diclofenac, ibuprofen, ketoprofen, and piroxicam—are as effective as their oral/systemic counterparts in treating localized osteoarthritis.13
A 2015 review of safety studies involving 2,403 subjects examined administration of topical vs. oral NSAIDs in treating osteoarthritis of the knee. Investigators found that the two modalities “demonstrated similar efficacy,” but patients taking the oral drug experienced gastrointestinal side effects while patients in the topical arms did not.14
Another larger review15, which included data from patient surveys, concluded that “topical and oral NSAIDs demonstrate an equivalent effect on knee pain over 1 year of treatment, with fewer adverse events due to lower systemic absorption of topical NSAIDs compared with oral NSAIDs.” This study also reported that fewer patients changed topical medications due to adverse events, compared with patients taking oral NSAIDS, and that three-quarters of subjects preferred the oral dosage form. As an added benefit, patients requiring both topical and oral forms of NSAIDs for osteoarthritis were able to reduce oral dosing of their NSAID by 40%, thus further reducing the potential for experiencing side effects.
Capsaicin and Salicylates
Many over-the-counter topical pain treatments are based on “natural” or non-pharmaceutical active ingredients. These products, which are effective but undergo no significant systemic distribution, include counter-irritant or “rubefacients,” eg, menthol, camphor, or salicylates.16 Rubefacients cause redness and a sensation of warmth, and promote healing by dilating capillaries in the skin.17
Capsaicin and salicylates are two additional topical agents of interest, both of which may have multiple modes of action. Derived from chili peppers, capsaicin is a counter-irritant. But unlike similarly acting agents like camphor, it exhibits significant pharmacologic activity, specifically reducing pain by desensitizing sensory afferent18 neurons. Capsaicin has been used to treat several types of nerve pain, gastropathy, post-mastectomy pain, pruritus, overactive bladder, and both chemotherapy- and radiation-induced mucositis.
Derived from willow tree bark and chemically related to aspirin, salicylates also work primarily as counter-irritants, producing the sensation of heat or cold. Very little salicylate penetrates into systemic circulation, so the inhibition of pain-mediating cyclooxygenase intermediates typical of aspirin most likely does not contribute to pain relief. However, salicylates do penetrate into several skin layers, where they are hydrolyzed to salicylic acid. Salicylates may inhibit pro-inflammatory transcription factors and kinases, but their exact mode of action has not been elucidated.19
Cannabinoids: A Fresh Look
Cannabinoids have been known, in one form or another, for centuries. But their pharmacologic activity has only recently been appreciated. Like NSAIDs, cannabinoids show significant activity as both oral and topical agents. Depending on their structure, cannabinoids act on one or both cannabinoid receptor types: CB1 receptors, found primarily in somatic cells20, and CB2 receptors located mainly in immune cells.21
Like most plants, particularly those with medicinal value, cannabis is a virtual organic synthesis engine churning out more than 550 distinct chemical structures and approximately 100 cannabinoids.22 Among the non-psychotropic cannabinoids cannabidiol (CBD) stands out for its in vivo activity. CBD acts as an agonist or antagonist to more than 80 distinct biological receptors, including enzymes, ion channels/receptors, G-protein coupled receptors, transporter proteins, and nuclear receptors. Many of these molecules participate in biological pathways involved in pain, inflammation, and mood.23 Classically, wide-ranging activity of this type suggests potential therapeutic utility, either for the native compound or through chemical modification.
The inherent safety of non-pharmaceutical topical agents, including CBD, also suggests the potential to combine them to achieve treatment synergy. For example, our physical therapy practice uses a commercial topical pain cream containing methyl salicylate, menthol, and camphor at 12.5%, 7.4%, and 3.2%, respectively. We also use a product containing CBD and menthol plus other “generally regarded as safe” (GRAS) compounds. This is applied normally in conjunction with instrument assisted soft tissue manipulation (IASTM), or in conjunction with joint mobilization/manipulation. It often reduces sensitivity to movement and enhances the pain modulation after the manual therapy treatment. The CBD-based cream used in our practice is sold only through healthcare practices and clinics.
Based on positive results with patients in our clinic, we have a keen interest in further studying topical pain relief products containing CBD alone or combined with other GRAS actives and inactive ingredients.
PRODUCT RESOURCE: Pain Modalities
These companies offer products in different pain modalities that physical therapists can use for pain management and relief:
Battle Creek Equipment Co
CranioCradle
LightForce Therapy Lasers
Mettler Electronics Corp
Multi Radiance Medical
Pivotal Health Solutions
www.pivotalhealthsolutions.com
Southwest Technologies Inc
Thought Technology
Zimmer MedizinSystems
Clinical Evidence for CBD in Topicals
Large, randomized, double-blind, placebo-controlled clinical trials, the gold standard for clinical acceptance of new products, exist for CBD. However, studies tend to be small and do not always examine CBD alone, but in combination with other cannabinoids. Many studies combine CBD with THC, the major psychoactive component of cannabis, leaving open the question of which compound is responsible for the therapeutic effect. Such studies may advance clinical care, but they achieve this without mechanistic understanding. For example, more than half of patients receiving a mixture of CBD and three other cannabinoids (excluding THC) to treat severe, chronic pain were able to reduce or eliminate opioids.24
Recognizing the inherent uncertainty in such studies, Australian researchers undertook the largest, most comprehensive test of oral CBD alone to date. Their dose-ranging study of CBD in advanced cancer patients undergoing palliative care, is ongoing.25 These investigators have launched a parallel study on CBD + psychoactive delta-9 THC, which is also still in progress.26 With these studies as their reference point the same authors published a third article, on overcoming recruitment hurdles for future palliative care studies, which is expected to streamline future studies of CBD and other topical agents as well.27
Note that the studies mentioned so far all involve oral, not topical, CBD administration. Experience with oral-topical switches (particularly NSAIDs), combined with CBD’s diverse biological effects, provides a rationale or expectation that this agent could be effective topically as well, a supposition supported by animal studies.
A study of topical CBD gel alone, at various concentrations, in treating a rat knee osteoarthritis model found that treated animals recovered to near-baseline functioning. Perhaps as significantly, plasma CBD concentrations were linear with respect to loading dosage. The authors concluded that “topical CBD application has therapeutic potential for relief of arthritis pain-related behaviors and inflammation without evident side-effects.”28
CBD Monotherapy
Clinical studies of topical CBD monotherapy for treating pain are now emerging as well, with encouraging results from several high-quality studies. One crossover trial of commercial CBD oil in 29 patients with moderate pain reported that transdermal application achieves “significant improvement in pain and other disturbing sensations in patients with peripheral neuropathy,” that treatment was well tolerated, and may provide “a more effective alternative” to standard medications.29
Similarly, a double-blind, placebo-controlled study in 60 patients with myofascial pain compared topical CBD applied twice daily to placebo. Muscle activity was measured on days 0 and 14. When results were unblinded, 14 subjects receiving CBD showed decreased masseter muscle activity of 11% (right masseter muscles) and 13% (left), while the decrease in the control group averaged 1.7%; pain intensity also decreased in the treatment group by 70.2%, compared with just under 10% for the controls, a result that is highly significant.30
Another crossover study examining the effectiveness of topical CBD in treating neuropathic pain of the lower extremities, found “a statistically significant reduction in intense pain, sharp pain, cold and itchy sensations in the CBD group,” and no adverse events. The authors concluded that transdermal CBD “may provide a more effective alternative compared to other current therapies in the treatment of peripheral neuropathy.”31
More recently, a small phase 2 study on thumb basal joint arthritis treated 18 patients with a formulation of CBD oil in shea butter, versus shea butter alone. CBD treatment resulted in significant improvements from baseline, compared with placebo, in Visual Analog Scale Pain, Single Assessment Numeric Evaluation scores, and Disabilities of the Arm, Shoulder, and Hand scores, plus improvements in range of motion, grip, and pinch strength, with no significant adverse events reported.32
CBD Warrants Further Consideration
These studies, and my personal experience in treating patients with a variety of conditions, suggest that additional high-quality clinical investigation is warranted to support wider use of topical agents for the relief of mild- to moderate pain. The need is particularly urgent in situations where systemic distribution and side effects must be avoided, or when opioids or other addictive treatments are the patient’s only option for relief.
The safety and effectiveness of oral CBD, and the vast literature on oral-to-topical formulation switches, provide further hope that caregivers will adopt topical CBD products appropriately. Interestingly, satisfaction with topical CBD preparations is already quite high. One study found that, among patients undergoing palliative treatment for pain, 24% already used CBD, with topical administration being the most common route of delivery.33
CBD’s multifaceted interactions with approximately 80 biological receptors, many of which are involved in pain and inflammation, provides an even more compelling rationale for further study. CBD, particularly as a topical agent, is safe and lacks abuse potential, but inconsistent and unregulated manufacturing practices have led to inconsistent product quality. Rehabilitation therapists should therefore limit their use of topical CBD to products produced under current Good Manufacturing Practices, the same standard applied to FDA-approved medications.34
Finally, topical CBD has the potential to enhance the value of rehabilitation programs to patients, especially when combined with manual therapy, and the potential to provide these benefits safely and cost effectively.
Erson Religioso III, DPT, MS, MTC, CFC, CertMDT, CertMST, CNPT, FAAOMPT, is a Doctor of Physical Therapy and fellowship-trained entrepreneur, blogger, and sought after lecturer in the topic of Modern Manual Therapy – The Eclectic Approach. He has a physical therapy practice called EDGE Rehab and Sport Science, located in the Buffalo, NY, area where he specializes in TMD, headaches, spinal care, chronic pain, and treating runners and gymnasts. He graduated from D’Youville College in 1998 with a dual BS/MS in Physical Therapy and further specialized with a Manual Therapy Certificate and Doctor of Physical Therapy from the University of St. Augustine in 2000. “Modern Manual Therapy – The Eclectic Approach,” is Religioso’s line of seminars for clinicians that are taught online and in live venues around the world. Seminar topics include manual therapy, patient education, blood flow restriction therapy/training, barbell therapy, and nutrition for clinicians.
References
1 Ruth L Chimenti, Laura A Frey-Law, Kathleen A Sluka, A Mechanism-Based Approach to Physical Therapist Management of Pain, Physical Therapy, Volume 98, Issue 5, May 2018, Pages 302–314, https://doi.org/10.1093/ptj/pzy030
2 Miller DL, Smith NB, Bailey MR, et al. Overview of therapeutic ultrasound applications and safety considerations. J Ultrasound Med. 2012;31(4):623-34.
3 Karatzanos E, Gerovasili V, Zervakis D, et al. Electrical muscle stimulation: an effective form of exercise and early mobilization to preserve muscle strength in critically ill patients. Crit Care Res Pract. 2012;2012:432752. doi:10.1155/2012/432752
4 Koutsioumpa E, Makris D, Theochari A, et al. Effect of Transcutaneous Electrical Neuromuscular Stimulation on Myopathy in Intensive Care Patients. Am J Crit Care. 2018;27(6):495-503. doi:10.4037/ajcc2018311
5 Rahbar M, Ranjbar Kiyakalayeh S, Mirzajani R, Eftekharsadat B, Dolatkhah N. Effectiveness of acromioclavicular joint mobilization and physical therapy vs physical therapy alone in patients with frozen shoulder: A randomized clinical trial. Clin Rehabil. 2022 May;36(5):669-682. doi: 10.1177/02692155211070451. Epub 2021 Dec 29. PMID: 34964679
6 Grana WA. Physical agents in musculoskeletal problems: heat and cold therapy modalities. Instr Course Lect. 1993;42:439-42. PMID: 8463693.
7 Handoll HH, Elliott J. Rehabilitation for distal radial fractures in adults. Cochrane Database Syst Rev. 2015 Sep 25;2015(9):CD003324. doi: 10.1002/14651858.CD003324.pub3. PMID: 26403335; PMCID: PMC9250132.
8 Crawford C, Boyd C, Paat CF, et al. The Impact of Massage Therapy on Function in Pain Populations-A Systematic Review and Meta-Analysis of Randomized Controlled Trials: Part I, Patients Experiencing Pain in the General Population. Pain Med. 2016;17(7):1353-1375. doi:10.1093/pm/pnw099
9 Jorge LL, Feres CC, Teles VE. Topical preparations for pain relief: efficacy and patient adherence. J Pain Res. 2010;4:11-24. Published 2010 Dec 20. doi:10.2147/JPR.S9492
10 Derry S, Wiffen PJ, Kalso EA, et al. Topical analgesics for acute and chronic pain in adults – an overview of Cochrane Reviews. Cochrane Database Syst Rev. 2017;5(5):CD008609. Published 2017 May 12. doi:10.1002/14651858.CD008609.pub2.
11 Martin C. et al. Controlled-release of opioids for improved pain management. Materials Today, 2016;19(9). doi: 10.1016/j.mattod.2016.01.016.
12 Leppert, Wojciech & Malec-Milewska, Małgorzata & Zajączkowska, Renata & Wordliczek, Jerzy. (2018). Transdermal and Topical Drug Administration in the Treatment of Pain. Molecules. 23. 681. doi: 10.3390/molecules23030681.
13 Zeng C, Doherty M, Persson MSM et al. Comparative efficacy and safety of acetaminophen, topical and oral non-steroidal anti-inflammatory drugs for knee osteoarthritis: evidence from a network meta-analysis of randomized controlled trials and real-world data. Osteoarthritis Cartilage. 2021 Sep;29(9):1242-1251. doi: 10.1016/j.joca.2021.06.004.
14 Klinge SA, Sawyer GA (2013) Effectiveness and Safety of Topical versus Oral Nonsteroidal Anti-inflammatory Drugs: A Comprehensive Review, The Physician and Sportsmedicine, 41:2, 64-74, DOI: 10.3810/psm.2013.05.2016
15 Rannou F, Pelletier J-P, Martel-Pelletier J (2016) Efficacy and safety of topical NSAIDs in the management of osteoarthritis: Evidence from real-life setting trials and surveys. Seminars in Arthritis and Rheumatism, 45:4. doi: 10.1016/j.semarthrit.2015.11.007.
16 Barkin RL. The pharmacology of topical analgesics. Postgrad Med. 2013 Jul;125(4 Suppl 1):7-18. doi: 10.1080/00325481.2013.1110566911. PMID: 24547599.
17 Matthews P, Derry S, Moore RA, McQuay HJ. Topical rubefacients for acute and chronic pain in adults. Cochrane Database Syst Rev. 2009;(3):CD007403. Published 2009 Jul 8. doi:10.1002/14651858.CD007403.pub2.
18 Chang A, Rosani A, Quick J. Capsaicin. [Updated 2022 May 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459168/
19 Wong, J. (2010). Topical salicylates. In R. Sinatra, J. Jahr, & J. Watkins-Pitchford (Eds.), The Essence of Analgesia and Analgesics (pp. 410-412). Cambridge: Cambridge University Press. doi:10.1017/CBO9780511841378.103.
20 Pacher P, Bátkai S, Kunos G. The endocannabinoid system as an emerging target of pharmacotherapy. Pharmacol Rev. 2006;58(3):389-462. doi:10.1124/pr.58.3.2.
21 Marchand J, Bord A, Pénarier G, Lauré F, Carayon P, Casellas P. Quantitative method to determine mRNA levels by reverse transcriptase-polymerase chain reaction from leukocyte subsets purified by fluorescence-activated cell sorting: application to peripheral cannabinoid receptors. Cytometry. 1999 Mar 1;35(3):227-34. doi: 10.1002/(sici)1097-0320(19990301)35:3<227::aid-cyto5>3.0.co;2-4. PMID: 10082303.
22 Rock EM, Parker LA. Constituents of Cannabis Sativa. Adv Exp Med Biol. 2021;1264:1-13. doi: 10.1007/978-3-030-57369-0_1. PMID: 33332000.
23 Mlost J, Bryk M, Starowicz K. Cannabidiol for Pain Treatment: Focus on Pharmacology and Mechanism of Action. International Journal of Molecular Sciences. 2020; 21(22):8870. https://doi.org/10.3390/ijms21228870.
24 Capano A, Weaver R, Burkman E. Evaluation of the effects of CBD hemp extract on opioid use and quality of life indicators in chronic pain patients: a prospective cohort study. Postgrad Med. 2020 Jan;132(1):56-61. doi: 10.1080/00325481.2019.1685298. Epub 2019 Nov 12. PMID: 31711352.
25 Good P, Haywood A, Gogna G, Martin J, Yates P, Greer R, Hardy J. Oral medicinal cannabinoids to relieve symptom burden in the palliative care of patients with advanced cancer: a double-blind, placebo controlled, randomised clinical trial of efficacy and safety of cannabidiol (CBD). BMC Palliat Care. 2019 Dec 6;18(1):110. doi: 10.1186/s12904-019-0494-6. PMID: 31810437; PMCID: PMC6898965
26 Hardy J, Haywood A, Gogna G, Martin J, Yates P, Greer R, Good P. Oral medicinal cannabinoids to relieve symptom burden in the palliative care of patients with advanced cancer: a double-blind, placebo-controlled, randomised clinical trial of efficacy and safety of 1:1 delta-9-tetrahydrocannabinol (THC) and cannabidiol (CBD). Trials. 2020 Jul 6;21(1):611. doi: 10.1186/s13063-020-04541-6. PMID: 32631447; PMCID: PMC7336664.
27 Olson RE, Smith A, Huggett G, Good P, Dudley M, Hardy J. Using a qualitative sub-study to inform the design and delivery of randomised controlled trials on medicinal cannabis for symptom relief in patients with advanced cancer. Trials. 2022 Sep 5;23(1):752. doi: 10.1186/s13063-022-06691-1. PMID: 36064621; PMCID: PMC9444122.
28 Hammell DC, Zhang LP, Ma F, Abshire SM, McIlwrath SL, Stinchcomb AL, Westlund KN. Transdermal cannabidiol reduces inflammation and pain-related behaviours in a rat model of arthritis. Eur J Pain. 2016 Jul;20(6):936-48. doi: 10.1002/ejp.818. Epub 2015 Oct 30. PMID: 26517407; PMCID: PMC4851925.
29 Xu DH, Cullen BD, Tang M, Fang Y. The Effectiveness of Topical Cannabidiol Oil in Symptomatic Relief of Peripheral Neuropathy of the Lower Extremities. Curr Pharm Biotechnol. 2020;21(5):390-402. doi: 10.2174/1389201020666191202111534. PMID: 31793418.
30 Nitecka-Buchta A, Nowak-Wachol A, Wachol K, Walczyńska-Dragon K, Olczyk P, Batoryna O, Kempa W, Baron S. Myorelaxant Effect of Transdermal Cannabidiol Application in Patients with TMD: A Randomized, Double-Blind Trial. J Clin Med. 2019 Nov 6;8(11):1886. doi: 10.3390/jcm8111886. PMID: 31698733; PMCID: PMC6912397.
31 Xu DH, Cullen BD, Tang M, Fang Y. The Effectiveness of Topical Cannabidiol Oil in Symptomatic Relief of Peripheral Neuropathy of the Lower Extremities. Curr Pharm Biotechnol. 2020;21(5):390-402. doi: 10.2174/1389201020666191202111534. PMID: 31793418.
32 Heineman JT, Forster GL, Stephens KL, Cottler PS, Timko MP, DeGeorge BR Jr. A Randomized Controlled Trial of Topical Cannabidiol for the Treatment of Thumb Basal Joint Arthritis. J Hand Surg Am. 2022 Jul;47(7):611-620. doi: 10.1016/j.jhsa.2022.03.002. Epub 2022 May 28. PMID: 35637038.
33 Highet BH, Lesser ER, Johnson PW, Kaur JS. Tetrahydrocannabinol and Cannabidiol Use in an Outpatient Palliative Medicine Population. Am J Hosp Palliat Care. 2020 Aug;37(8):589-593. doi: 10.1177/1049909119900378. Epub 2020 Jan 27. PMID: 31986898.
34 Fitzcharles MA, Clauw DJ, Hauser W. A cautious hope for cannabidiol (CBD) in rheumatology care. Arthritis Care Res (Hoboken). 2020 Mar 7. doi: 10.1002/acr.24176. Epub ahead of print. PMID: 32144889.