Microchips meets the laws of physics for modern solutions to pain problems.
By Frank Long, MS
For more than 100 years physical therapists have used manual therapy techniques to relieve pain symptoms and restore function. The fact that manual techniques have enjoyed such a long shelf life does not suggest that today’s advanced technologies cannot improve on what hands alone accomplish. In fact, pain management technologies such as laser light, ultrasound waves, and biofeedback help therapists gain new ground each day in an old battle. Before purchasing one of these devices, however, therapists should learn the healing mechanisms behind each modality and understand the benefits each provides. Here are the must-know buying tips.
Healing Lights
Few things shout, “State of the art,” quite like lasers. Science fiction helped bring the power of lasers into the public consciousness in the 1950s, but in today’s world it is medical lasers that generate buzz by shutting down pain symptoms. Class IV lasers in particular are known for putting the pain-relieving benefits of low-level laser therapy into clinicians’ hands.
Class IV lasers are characterized by having output powers greater than 500 mW or 0.5 Watts. They are approved by the FDA for use with a number of conditions that range from treating sprains and strains to promoting joint healing and reducing swelling. Class IV lasers use specific light wavelengths to penetrate tissues and speed up cell metabolism. This, in turn, promotes healing through a process called photobiomodulation, which stimulates tissue repair and growth.
Power and Productivity
At the heart of therapeutic laser treatment is the power of the laser itself, which means therapists must understand the power rating of the device and how to use it so they get the best outcomes. Mark L. Callanen, PT, DPT, OCS, offers these helpful tips for understanding the importance of laser power in the 2019 August/September Physical Therapy Products:
“Remembering that energy applied (Joules) = power (Watts) x time (seconds), recent research is showing that applying energy to tissue with high-power lasers impacts tissue differently than applying an equal number of Joules with low-power lasers. This has been shown in studies that compared the two regarding knee OA1 and plantar fasciitis,2 where high-power laser provided more pain relief and better functional outcomes, comparatively. Other studies looking at high-power laser versus placebo have also shown favorable outcomes regarding shoulder impingement3 and low back pain.4
“Most therapeutic lasers impact pain via PBM’s influence on reducing inflammation around peripheral nerve endings.5,6 However, high-power lasers can reduce pain in minutes by delivering higher irradiance levels to nerve tissue.7,8
“This is an important differentiator between high- and low-power lasers. Quick pain relief requires higher irradiance to elicit temporary neuroplastic changes at the neuron. These changes slow the conduction velocity and reduce the amplitude of compound action potentials of both C and A-delta sensory nerves for approximately 24 hours.8,9 These higher irradiances are extremely difficult to achieve in vivo with lower-power devices.”
Shopping for Lasers
As a pain reliever laser therapy offers the desirable advantage of being non-addictive and non-invasive. It also has very few contraindications. In the physical therapy market several manufacturers offer laser devices for therapeutic treatment, including Zimmer MedizinSysteme and LiteCure Medical.

OptonPro
Zimmer MedizinSysteme, Irvine, Calif
Class IV
25 Watts, 3 Wavelengths
www.ZimmerUSA.com
Ultrasound for Physical Therapy
Like manual therapy, hot packs have had a long run as a pain management modality as a simple and affordable tool, yet a tool strictly limited to superficial treatment. In contrast, ultrasound uses high-frequency waves to reach deep tissues, causing them to vibrate and heat up. This effect can be used to relax muscles and reduce pain, but ultrasound can also be used to break down scar tissue, which helps improve elasticity and range of motion.
Programmable for Perfection
The effectiveness of ultrasound devices has a great deal to do with how the units are programmed. This means therapists who use ultrasound devices must determine whether the tissue that requires treatment is superficial (1-2 cm) or deep (2-5 cm), and adjust frequency, intensity, and duration accordingly. A properly programmed ultrasound device will need to be matched with a sound head of the correct size. Treatment across a large area such as the quadriceps or piriformis will require a larger sound head, while treatment for a specific tendon in the hand will require a smaller sound head.
Don’t Forget the ERA
The effective radiating area (ERA) is a vital factor to consider when purchasing an ultrasound unit. This is because typically the greatest amount of energy delivered by an ultrasound device is concentrated toward the center of the sound head, and it becomes weaker toward the edge. As a result, the ERA for an ultrasound unit will be smaller than the actual size of the sound head. In terms of the beam itself, an ultrasound unit that has a large ERA will produce a collimated beam that spreads minimally while a small ERA will produce a beam that is more divergent.
Since ultrasound waves cannot pass through air, they require a coupling medium to seal the gap between skin and the ultrasound probe. In physical therapy applications this medium oftentimes is a gel. The gel increases the transmission of ultrasound waves and helps the therapist to move the probe smoothly on the skin.
Shopping for Ultrasound
Therapy clinics that need a versatile ultrasound unit for portable applications or for use in the office have several choices. Professional ultrasound devices for physical therapists are available from sources that include Mettler Electronics and Dynatronics Corp.

LightForce EXPi
LiteCure Medical, New Castle, Del
Class IV
25 watts, 2 wavelengths
www.lightforcelasers.com

The Sonic*Tool
Mettler Electronics Corp, Anaheim, Calif
Combines IASTM and therapeutic ultrasound.
Attaches to a 5cm2 applicator.
www.mettlerelectronics.com

Solaris Plus
Dynatronics Corp, Salt Lake City
Up to 6 waveforms and 5 channels of stim.
Soundhead sizes 2cm2, 5cm2, 10cm2
www.dynatronics.com
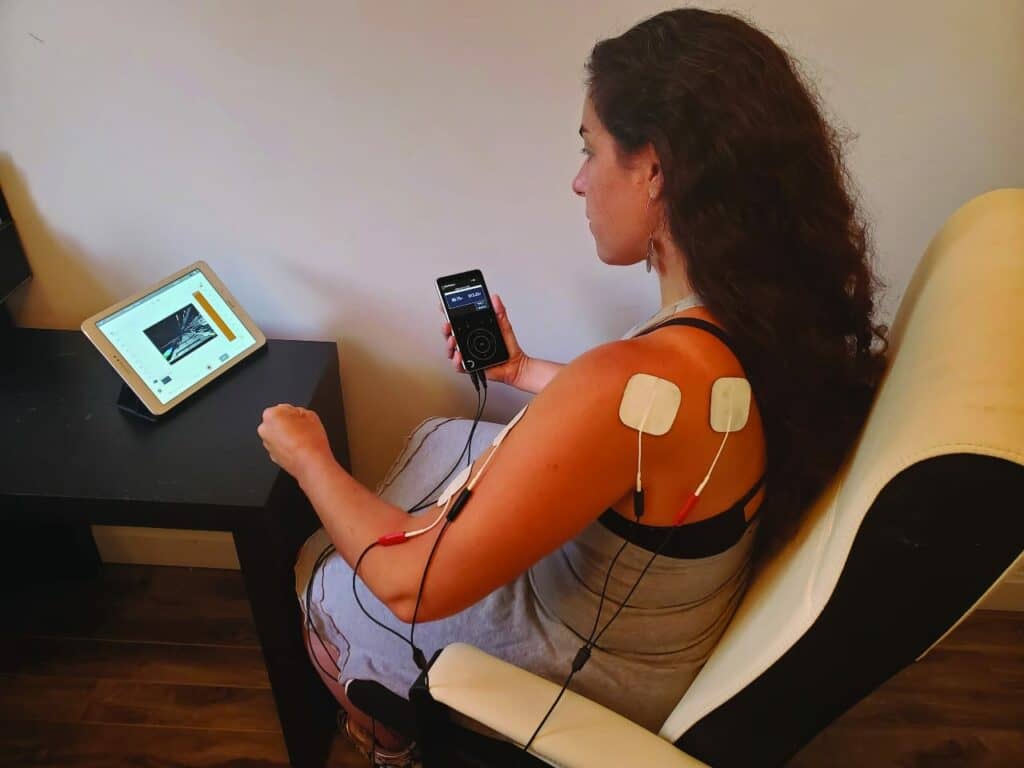
MyOnyx
Thought Technology Ltd, Montreal, Canada
Portable, rechargeable, and wireless.
MyOnyx smartphone app works as a remote control for MyOnyx hardware.
www.thoughttechnology.com
Biofeedback for Body and Mind
Born in the 20th century, biofeedback is a child of the modern age whose applications continue to unfurl. Biofeedback is applied as a mind-body technique clinicians can use to help individuals modify their physiology. It requires state-of-the-art equipment that can convert physiological signals into actionable cues that patients can use to control their physiology through self-regulation. Used correctly with a patient’s active participation, biofeedback can generate data that help improve an individual’s physical, emotional, and mental health.
Biofeedback for Pain Treatment
Surface electromyography (sEMG) is a key element of biofeedback that helps measure muscle activation, teaches relaxation, or can be used to assist with fine motor control. In the article, “Biofeedback in medicine: who, when, why, and how?” published in Mental Health in Family Medicine,10 chronic pain, spasmodic torticollis, and temporomandibular joint dysfunction are three disorders for which biofeedback can be used to improve outcomes.
Biofeedback is not considered treatment but rather a type of training; a specialized way to induce patients to see inside their bodies and regulate their physiology toward a positive outcome. The technology is surprisingly versatile. While it has become known as a modern method for addressing pain symptoms, biofeedback can also be helpful in stroke rehabilitation11 and as a performance-enhancement strategy in athletes.12,13,14
Shopping for Biofeedback
Biofeedback devices are available on the retail market, but there is also at least one source for clinical-level biofeedback appropriate for physical therapist use, which is Montreal-headquartered company Thought Technology Ltd. PTP
Frank Long, MS, is the former editorial director of Physical Therapy Products. For more information, contact [email protected].
References
- Wyszynska J, Bal-Bochenska M. Efficacy of high-intensity laser therapy in treating knee osteoarthritis: a first systematic review. Photomed Laser Surg. 2018;36(7):343-353.
- Ordahan B, Karahan AY, Kaydok E. The effect of high-intensity versus low-level laser therapy in the management of plantar fasciitis: a randomized clinical trial. Lasers Med Sci. 2018 Aug;33(6):1363-1369.
- Elsodany AM, Alayat MSM, Ali MME, Khaprani HM. Long-term effect of pulsed Nd:YAG laser in the treatment of patients with rotator cuff tendinopathy: a randomized controlled trial. Photomed Laser Surg. 2018;36(9):506-513.
- Vallone F, Benedicenti S, Sorrenti E, Schiavetti I, Angiero F. Effect of diode laser in the treatment of patients with nonspecific chronic low back pain: a randomized controlled trial. Photomed Laser Surg. 2014;32(9):490-494.
- Cotler H, Chow RT, Hamblin MR, Carroll J. The use of low level laser therapy (LLLT) for musculoskeletal pain. MOJ Orthop Rheumatol. 2015;2(5).
- Huang YY, Chen AC, Carroll JD, Hamblin MR. Biphasic dose response in low level light therapy. Dose Response. 2009;7(4):358-383.
- Enwemeka CS. Intricacies of dose in laser phototherapy for tissue repair and pain relief. Photomed Laser Surg. 2009;27(3):387-393.
- Chow R, Armati P, Laakso EL, Bjordal JM, Baxter GD. Inhibitory effects of laser irradiation on peripheral mammalian nerves and relevance to analgesic effects: a systematic review. Photomed Laser Surg. 2011;29(6):365-381.
- Holanda VM, Chavantes MC, Wu X, Anders JJ. The mechanistic basis for photobiomodulation therapy of neuropathic pain by near infrared laser light. Lasers Surg Med. 2017 Jul;49(5):516-524.
- Frank DL, Khorshid L, Kiffer JF, Moravec CS, McKee MG. Biofeedback in medicine: who, when, why and how?. Ment Health Fam Med. 2010;7(2):85-91.
- Kim JH. The effects of training using EMG biofeedback on stroke patients upper extremity functions. J Phys Ther Sci. 2017;29(6):1085-1088. doi: 10.1589/jpts.29.1085
- Brown DJ, Fletcher D. Effects of psychological and psychosocial interventions on sport performance: a meta-analysis. Sports Med. 2016;47(1):77–99.
- Keilani M, Hasenöhrl T, Gartner I, Krall C, Fürnhammer J, Cenik F, Crevenna R. Use of mental techniques for competition and recovery in professional athletes. Wien Klin Wochenschr. 2016;128:315–319.
- Pusenjak N, Grad A, Tusak M, Leskovsek M, Schwarzlin R. Can biofeedback training on psychophysiological responses enhance athletes’ sports performance? a practitioner’s perspective. Phys Sportsmed. 2015;43(3):287–289.




