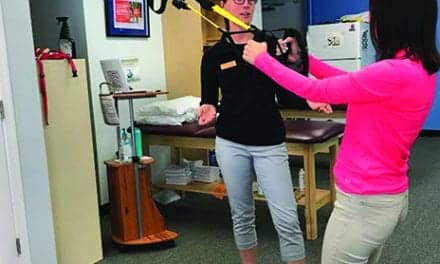
Devin Breedon, RDN, LD, counsels a patient at HealthSouth Rehabilitation Hospital of Ocala. Breedon says functional decline may correlate with poor nutrition and hydration, which makes communicating with a dietitian to promote a shared goal a necessary part of the rehab process.
Who doesn’t want the best patient outcomes? Daily as care providers, clinicians emphasize a goal to promote the best patient outcomes, but how often is that goal met? In the world of physical therapy, providers work toward increasing independence, strength and mobility, but all too often, setbacks impede progression and delay achieving these goals. Nutrition may play a significant role in patient stability, which in turn increases productivity of a therapy session. A therapist can utilize a registered dietitian in hopes of increasing productivity of therapy to maximize patient potential and meet goals.
Dietitians in PT
A dietitian’s role in the recovery of a patient may not be clear in the world of physical therapy. As a dietitian, I assess and treat patients with complex nutrition-related conditions, some of which directly affect the physical function of an individual. These conditions include well-known diseases such as diabetes, obesity, malnutrition, osteoporosis and anemia. If a patient is not nutritionally stable, their therapeutic potential is squandered. A patient’s non-compliance with diet, a lack of oral intake, altered nutrition-related labs, altered gastrointestinal function, decreased muscle mass or poor hydration may result in a less than ideal therapy candidate.
A dietitian’s ability to assess and treat these conditions therefore becomes more important. My goal is to ensure patients are consuming the necessary energy and fluid to manage underlying medical conditions as well as progress in therapy. The dietitian may address this goal by providing a therapeutic diet, oral nutritional supplements, medications or vitamins/minerals to promote optimal nutrition. Many nutrition-related medical conditions, if not treated, lead to functional decline over time. I, too, must understand the role of nutrition in physical function. A major component of a dietitian’s plan of care is the promotion and encouragement to participate in therapy as well as the ability to explain the benefits of exercise as well as the ill effects of a sedentary lifestyle. Unfortunately, some nutrition-related concerns may not come to light for a dietitian unless purposeful communication occurs. Physicians or nurses consult a dietitian by default, but as part of a rehabilitation team, a therapist has the ability to communicate nutrition-related concerns as well as promote nutrition goals. This is where the communication between the therapist and dietitian is crucial.

Working as part of the therapy team, Devin Breedon, RDN, LD, and a physical therapist discuss nutrition with a patient prior to discharge. Breedon notes that because therapists spend more time with patients, they may be able to identify a change in nutrition status before regularly scheduled follow up with a dietitian.
Know the patient’s diet
A physical therapist can play a significant role in the nutrition care of patients in rehabilitation. A decline in function may correlate with poor nutrition and hydration; therefore, communicating with a dietitian to promote a shared goal is a necessary part of the rehabilitation process. Initially, a therapist evaluates a patient’s ability to complete normal daily functions, something blunted by poor nutrition. When evaluating a patient, it may help to ask questions regarding meal intake or preferences, ability to feed self, hydration concerns, alterations to skin and any drastic weight changes over the past six to 12 months. It may be best practice to prevent deficiencies by addressing nutrition during initial visits with a patient, as inadequate nutrition and hydration may be pre-existing. As a patient progresses, or regresses, with therapy, it is important to be aware of meal and fluid intake and actively communicate with a dietitian to ensure the patient is maintaining proper nutrition to maximize outcomes in therapy. A therapist has the benefit of spending more time with a patient and may notice a change in nutrition status well ahead of a dietitian reassessment or follow up, being that a dietitian may only follow up every few days or not at all. This line of communication is important as a patient transitions home.
As part of the therapy team, I am involved in the transition home, which may include the assessment of barriers preventing patients from accessing or acquiring meals, some physical in nature. As these concerns arise, it is important that I discuss with a therapist in a timely manner to ensure patient is prepared following discharge. There may also be nutrition-related barriers at home that a dietitian may be able to address. These may include socioeconomic, education or food access concerns. If informed, a dietitian can work alongside a case/social worker to address any education or access concerns prior to discharge. As you can see, the relationship with a dietitian and therapists in promoting nutrition and hydration can be symbiotic and rewarding for both the patient and practitioners.
PT + Dietitian = ROI
The bond between nutrition and physical therapy is ever growing. When we work together to promote optimal outcomes while managing underlying medical concerns, we do the most for our patients. The benefit of working alongside a registered dietitian can help a therapist succeed, resulting in increased productivity and satisfaction, thus improving individual patient outcomes. The therapist can also benefit the dietitian in many different aspects of nutrition and see a significant return on this investment of time and energy. As we move into the future of rehabilitation, I challenge all therapists to improve their relationship with a dietitian to see the benefit of working alongside someone who specializes in nutrition, especially in the rehabilitation setting. Only together can we succeed, so let us succeed together.
Devin Breedon, RDN, LD, is a registered dietitian at HealthSouth Rehabilitation Hospital of Ocala. Devin graduated from Michigan State University with a bachelor’s degree in dietetics and completed a dietetic internship at Texas A&M-Kingsville. He has been providing nutritional counseling in a hospital and outpatient setting for six years, and specializes in geriatric and rehabilitative nutrition, working with a population that has extensive medical comorbidities including diabetes, heart disease and kidney disease. He plays an important role in the recovery and wellness of patients and participates as part of a team of other therapy professionals. Devin is also a member of the academy of Nutrition and Dietetics and the Florida Academy of Nutrition.