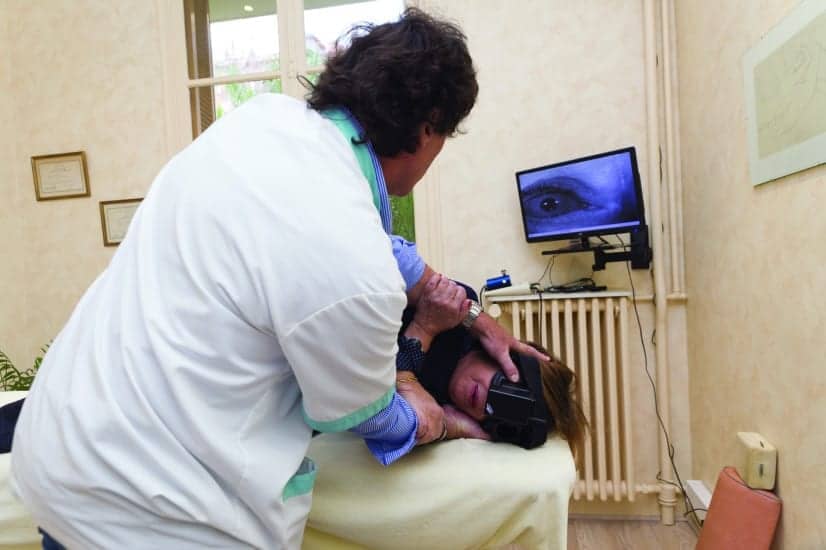
PHOTO CAPTION: Using Frenzel goggles, a therapist performs a vestibular exam on a dizzy patient. Tests that can be performed while a patient is wearing the goggles include Dix Hallpike, Roll test, gaze-evoked nystagmus, head impulse test, and head-shaking nystagmus.
By Emily Porter, PT, DPT
Dizziness is a common complaint heard in physical therapy practice. Whether it be in the acute care setting or an outpatient practice, there is an excellent chance that you will encounter a dizzy patient. While it may or may not be the primary reason they seek treatment, it is imperative that therapists are equipped to evaluate and determine if the patient is an appropriate candidate for vestibular rehab. Recent stats show that dizziness results in 6 million physician patients per year and affects 80% of older adults in outpatient settings.1 In fact, a recent study showed that 29-45% of individuals older than age 70 years have a vestibular disorder.2 The high incidence of vestibular dysfunction and ramifications, if left untreated, make the proper evaluation and treatment of dizziness of utmost importance.
Physical Therapy’s Unique Subset
Vestibular rehabilitation is a unique subset of physical therapy with the main goal of challenging the inner ear and restoring its normal function, if possible. At its very core, vestibular rehab is a therapeutic resource based on central mechanisms of neuroplasticity known as adaptation, habituation, and substitution. Adaptation is defined as repeated head movements while focusing on a target with the goal being to improve gaze stability with adaptation of the vestibular ocular reflex and development of compensatory saccadic eye movements.2 Substitution involves using the remaining sensory systems to assist with postural control. This becomes important when dealing with an inner ear loss of function that is unable to be corrected or one can use substitution principles in the beginning of treatment to increase function before adaptation occurs.3 Finally, habituation focuses on reducing the pathologic response to a provoking stimulus. These three principles are used together with the main goal of abolishing disabling symptoms through encouraging adaptation and repositioning of the vestibular system.4 Effective vestibular rehabilitation facilitates compensation after peripheral or central dysfunction has occurred with the primary goals being to decrease symptoms of dizziness and vertigo, improve balance, and return to previous level of function.
Identifying the Cause
Determining the cause of a patient’s dizziness can help determine the proper treatment plan. Common vestibular causes of dizziness include benign paroxysmal positional vertigo, post-concussion syndrome, unilateral or bilateral vestibular loss, Meniere’s disease, and migraine-associated vertigo. Central causes of dizziness may include multiple sclerosis, cerebrovascular accident, traumatic brain injury, brain tumor, and Parkinson’s disease. By hypothesizing the cause of dizziness, one can then move to treatment principles, deciding to implement habituation, substitution, or adaptation exercises. While one can perform a very thorough vestibular exam with little to no technology, there are several items on the market today to aid in diagnosing and treating vestibular disorders.

Frenzel Goggles and Nystagmus
Several manufacturers provide technologies that can help physical therapists evaluate and treat patients affected by dizziness disorders. One manufacturer, Interacoustics, Eden Prairie, Minn, offers the VisualEyes product line with a variety of software bundles and hardware options that expand the possibilities for functional assessment. The Interacoustics line includes the VisualEyes 505 Video Frenzel System, which provides a large volume of clinical data and can conduct a spontaneous nystagmus test utilizing a nystagmus detection algorithm.
Another product that can be used to evaluate the dizzy patient is Frenzel Nystagmus Goggles by Jedmed, located in St Louis. This particular pair is the optical version. Another type on the market is the VideoStar Frenzel goggles from Secure Health Inc in Fort Wayne, Ind. These can be extremely useful with evaluation of the dizzy patient. At the most basic level, the goggles consist of magnifying glasses and a lighting system. When placed on a patient with room lights darkened, nystagmus can become more easily seen as the patient’s eyes are magnified and illuminated and fixation is removed. This is very useful when determining which canal and ear is involved with benign paroxysmal positional vertigo (BPPV) or looking for gaze-evoked nystagmus in an acute hypofunction.
Tests that can be performed while the patient is wearing the goggles include Dix Hallpike, Roll test, gaze-evoked nystagmus, head impulse test, and head-shaking nystagmus. An advantage to purchasing the video goggles is having the ability to record nystagmus to watch repeatedly or compare to follow-up sessions. Direction-changing nystagmus from session to session is a red flag for central involvement. With conditions such as BPPV, the recording capability is beneficial as the intensity of nystagmus decreases as one repeatedly tests an ear due to the habituation principle. Likewise, sometimes nystagmus is very brief, and it can be beneficial to be able to watch repeatedly to ensure you have the correct pattern identified to inform your treatment plan.

Balance Testing Technology
Another helpful piece of technology is computerized dynamic posturography (CDP). The NeuroCom Smart Balance Master by Natus, from San Carlos, Calif, and the Bertec CDP/IVR, manufactured in Columbus, Ohio, are the systems most well-known and commonly seen in clinics. CDP is a method for quantifying balance and is most applicable in situations where balance needs to be followed quantitatively to demonstrate whether a disorder is getting better or worse, or to show disease progression over time. CDP is also a very effective objective measure to show response to treatment. The Sensory Organization Test is perhaps the most common of tests used and is an attempt to discern the somatosensory, visual, and vestibular contributions to one’s balance. An additional feature with both the Neurocom and Bertec systems is the ability to add on the vestibular ocular reflex (VOR) testing feature. The Dynamic Visual Acuity Test as well as the gaze stabilization test can be performed, adding quantitative and reliable measures to test VOR dysfunction and asymmetry. Aside from the testing features, both systems offer training modes where the therapist can manipulate the various settings, such as floor and wall responsiveness, to target patient-specific deficits. Newer models such as the Bertec system also allow you to portray various scenes inside the machine, such as a grocery store or mountain road, to further train one’s vestibular system.
[sidebar float=”left” width=”250″]Product Resources
The following companies offer products and services that can be helpful for vestibular rehabilitation:
Biodex Medical Systems
www.biodex.com
Hoggan Scientific LLC
www.hogganhealth.net
Interacoustics
www.interacoustics.com/us
Natus Medical Inc (NeuroCom)
www.onbalance.com
novel electronics
www.novelusa.com
Perry Dynamics Inc
www.perrydynamics.com[/sidebar]
Virtual Reality Intervention
While all the state-of-the-art technology is excellent, some may opt for a more budget-friendly option. Investing in a simple virtual reality goggle system can be a very effective and entertaining intervention for patients who have underlying vestibular systems. One example is the Sharper Image Bluetooth VR goggles, manufactured in Farmington Hills, Mich. There are hundreds of apps available to utilize with the goggles. A simple progression is to start the patient seated watching the video in a supported chair. Depending on symptom provocation, one can progress from sitting on an unstable surface, standing, and even walking. This is also an excellent exercise to give as a home exercise program depending on the patient’s technology availability.
Another very simple and cost-effective piece of technology is a laser. One example is the OPTP 594 SenMoCOR LED Laser/Headlamp manufactured in Minneapolis. This is used for joint position error testing, which is essential in post-concussion or cervicogenic dizziness treatment. The laser can also be used for cervical proprioception training. Many patients with vestibular dysfunction have underlying cervical proprioception issues that negatively affect their rehab potential. The skilled vestibular therapist can utilize even the simplest of technologies to address all layers of impairments potentially contributing to a patient’s report of dizziness.
Technology-Enhanced Treatment
Technology continues to advance, and new products are coming out every year. It is important to stay up to date on current research and evidence-based practice, utilizing the clinical practice guidelines as they are published. One can see how adding technology such as Frenzel goggles and computerized dynamic posturography only enhance one’s ability to efficiently diagnose and treat vestibular impairments. PTP
Emily Porter, PT, DPT, is a certified clinical vestibular therapist at ATI Physical Therapy in Clemson, SC, treating vestibular and neurological impairments. She also teaches in an integrated clinical reasoning course at Western Carolina University. Emily has a Doctorate of Physical Therapy from Western Carolina University in Cullowhee, NC. For more information, contact [email protected].
References
- Hall C, Heusal-Gillig L, Tusa R, Herdman S. Efficacy of gaze stability exercises in older adults with dizziness. JNPT. 2010;34:64-69. doi: 10.1097/NPT.0b013e3181dde6d8
- Iswasaki S, Tatsuya Y. Dizziness and imbalance in the elderly: age related decline in the vestibular system. Am J Otolaryngol. 2015;6,1:38-47. doi: 10.14336/AD.2014.0128
- Brodovsky J, Vnenchak M. Vestibular rehabilitation for unilateral peripheral vestibular dysfunction. Phys Ther. 2013;93:293-298. doi: 10.2522/ptj.20120057
- Ricci N, Aratani M, Dona F, et al. A systematic review about the effects of the vestibular rehabilitation in middle-age and older adults. Rev Bras Fisioter. 2010;14(5):361-71.