Lessons from Recovering COVID Patients Through Physical Therapy
by Seth Egge, PT
Imagine you catch COVID-19, a fear most people in the world have lived with for the past year. You begin to have difficulty breathing and go to the doctor for an assessment, where you’re informed you’ll have to stay in the hospital because you have an oxygen saturation level of below 85% and a resting heart rate of 110 that will not decrease. You’re placed on supplemental oxygen, and the next 9 days in the hospital are the most frightening of your life.
But there is more.
The thought of getting out of bed makes you breathless. Your legs are so weak, you can’t walk without a walker like your 80-year-old grandparent. Your heart races as you attempt to walk from the bed to the bathroom, feeling like you just ran a 400-yard dash. Finally, your vitals stabilize, and the doctor discharges you with a spirometer, walker, and prescriptions for your continued symptoms. When you check in with your primary care doctor, they prescribe physical therapy. The thought of going anywhere is exhausting, but you decide to attend and realize it may be the best decision of your life.
This story is one of many that I have heard as a physical therapist and one you are likely to encounter in the near future. As pandemic continues to ravage the U.S., patients suffering from the long-term effects of the virus are starting to arrive in our clinics with a multitude of conditions. We know this disease causes inflammation to the lining of the blood vessels resulting in a cascade of systemic compromise including blood clots, peripheral vascular disease, cardiovascular disease, and respiratory disease. The functional impairments caused by the disease can be as simple as generalized muscle weakness, shortness of breath and fatigue or as complex as POTS. These syndromes are manifesting from the disease and may be life altering.
Physical therapists are in the best position to help COVID patients recover and return to a higher quality of life. We’ve all learned a lot over the past year and have adapted our practice so we can be the providers of choice to assist these individuals. It is now our job to help those who will have to navigate living with the long-term effects of COVID. We are here for the patients looking for resources to return to their pre-COVID state of function.
Over the past 3 months I have encountered multiple PACER (Post-Acute COVID-19 Exercise Rehabilitation) patients that need physical therapy services. Below is a summary of my experiences (they are not absolutes). All clinical cases were unique, but they all had a few things in common: difficulty breathing, maintaining O2% saturation, elevated resting HR, generalized muscle weakness, and poor tolerance to daily activities. I share the objective tests and measures performed on my patients as ideas to get you thinking how you can help when you encounter these individuals.
Objective Tests to Consider
- Baseline Vitals
- Generalized UE/LE MMT
- Timed Up and Go: Testing for time, RPE, HR, RR, and 02%sat
- Tinetti or Berg Balance Assessment
- 5x Sit-to-Stand: Testing for time, RPE, HR, RR, and O2%sat
- 3-Minute YMCA Step Test: Testing time tolerated, RPE, HR, RR, and O2%sat
- 6-Minute Walk Test: Testing for time tolerated, RPE, HR, RR, and O2%sat
- Inflate Balloon Test: Measure circumference of balloon with one exhale to monitor forced Vital Capacity (FVC)
Initial Exam Findings
All patients were unable to complete the 6-minute walk test due to RPE, HR, RR, and 02%sat due to unsafe vitals. All struggled to complete 5x sit-to-stand and averaged less than 1 minute on the YMCA step test due to unsafe vitals.
Treatment Principles
- 8-week initial treatment plan of care, severity dependent
- 60-80 minutes sessions of therapeutic exercise and activities
- 10-30 minutes cardiovascular exercise
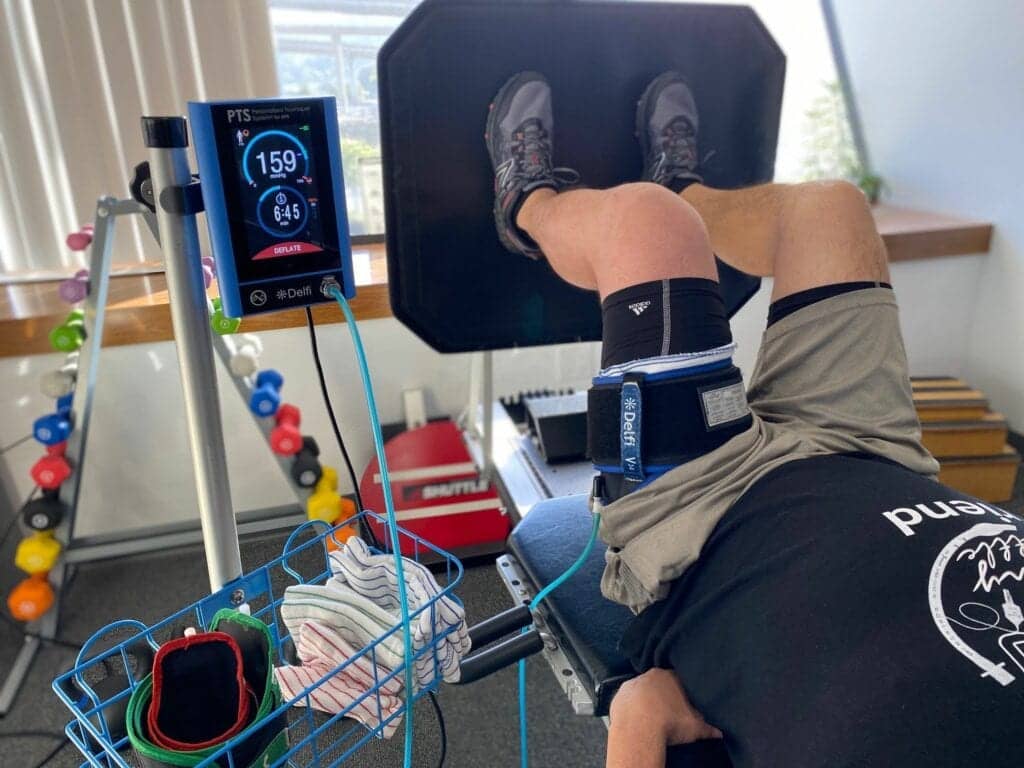
- Blood Flow Restriction
- 20-30 minutes functional strength training
- Blood Flow Restriction
- 10-20 minutes of breath training or meditation
- 10-30 minutes cardiovascular exercise
- Patients education focus on breath mechanics, meditation, and exercise principles
- Learn how to control breath to improve O2/C02 exchange efficiency
- Meditation to gain consciousness of body
- Interval exercise training principals
- Home Exercise Programs (HEP)
- Functional LE strengthening activities
- Generalized UE strengthening
- Diaphragmatic breathing
- Progressive Cardiovascular activity
Things to Consider
- Monitor vitals throughout visits for biofeedback
- Teach exercise principles and ensure patient safety
- Independent monitoring for long term management
- Reinforce importance of focused daily exercise and strength training
- Activities of Daily Living is not exercise
- Teach patients how to breathe
- Breathing is often taken for granted
- Review clinical safety parameters for exercise prescription
- ASCM “Guidelines for Exercise Testing and Prescription” for most updated guidelines
- Learn the principles of Blood Flow Restriction (BFR) to improve effectiveness of exercise intervention
Below is a list that will add to your knowledge of COVID-19, blood flow restriction training, breath mechanics training and ACSM guidelines. This by no means a comprehensive list and probably definitely not in MLA format, but it should lead you in the right direction.
Resources
- https://www.youtube.com/watch?v=mL7595lRqE0
- https://www.youtube.com/watch?v=mL7595lRqE0
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7443069/
- https://vimeo.com/showcase/7069923
- https://shiftadapt.com/product-tag/aob/
- https://www.healthline.com/health/breathing-exercise
- https://www.gloveworx.com/blog/breathing-exercises/
- https://www.acsm.org/read-research/books/acsms-guidelines-for-exercise-testing-and-prescription
Seth Egge, PT, is a clinic director at PRN San Diego in La Mesa, California. He treats patients who suffer from chronic low back and neck pain, craniofacial dysfunction, and complex upper and lower extremity disorders. Egge has a kinesiology degree from San Diego State University and a doctorate in physical therapy at the University of St. Augustine. For more information, contact [email protected].





