When it comes to equipment for children, one of the key factors to consider is their size. Pediatric LT equipment must be proportional to not only the child, but also the clinicians and trainers guiding the therapy.
By Andrea Behrman, PhD, PT, FAPTA
Nearly 1.3 million people in the United States live with a spinal cord injury (SCI), with about 20% of those injuries occurring in children younger than age 20 years. While rehab therapy for adult SCI has been well documented, pediatric SCI rehab presents unique challenges and requires different considerations than adults. Over the past 20 years, our understanding of neurorecovery in SCI, particularly in pediatric patients, has grown by leaps and bounds, thanks to ground-breaking neuroscience research.
[sidebar float=”right” width=”250″]Gait and Balance Technologies Get Patients Going: Technology Review
Gait and balance training can be an important part of rehabilitation for incomplete spinal cord injury, but it also factors significantly into functional recovery of individuals affected by stroke, traumatic brain injury, and neurological conditions. Following is a summary of technologies and manufacturers that strive to support gait and balance objectives that get patients going for discharge and beyond, including body weight support systems, gait mats, balance systems, specialized orthoses, stair trainers, and walkers.
Aretech, Ashburn, Va, offers the ZeroG Gait and Balance System, with customizable track designs, dynamic body-weight support, and fall protection set by range or velocity. Features include interactive games and balance programs, wearable sensors for validated outcome measures, treadmill integration, and patient harnesses with shaping handles. Training session data is stored in a HIPAA-compliant database to monitor progress.
Biodex Medical Systems Inc, Shirley, NY, manufactures Biodex Balance & Mobility to help position clinics as leaders in gait, mobility, balance, and fall risk screening and conditioning. In the face of today’s “Episode of Care” challenges, Biodex strives to equip clinics to treat complex patients, rehab them quickly, maximize staff, and provide safe discharge.
Bioness Inc, Valencia, Calif, is a provider of technologies designed to help people regain mobility and independence. Bioness solutions include external and implantable functional electrical stimulation (FES) systems, robotic systems, and software-based therapy programs providing functional and therapeutic benefits for individuals affected by pain, central nervous system disorders, and orthopedic injuries.
Clarke Health Care Products Inc, Oakdale, Pa, offers its Dynamic Stair Trainer with electronically adjustable steps, designed to motivate patients to climb steps faster. Remote controls adjust steps in 1-cm increments and height adjusts from flat to 6½ inches. Designed to be compact, it has a visual display to chart the patient’s progress and width-adjustable handrails. Entrance ramps that convert to steps are available.
GAITRite/CIR Systems Inc, Sparta, NJ, manufactures the GAITRite Portable Gait Analysis System, which automates measuring the temporal-spatial parameters of gait, balance, and stability. The electronic walkway is designed to roll out over a flat surface, require minimal setup, and quickly and easily collect accurate data. Connects to PC USB port; up to two cameras; use with/without assistive devices; standard clinical tests included with multiple report generation.
Gorbel Medical, Fishers, NY, offers the SafeGait 360° Balance and Mobility Trainer, a ceiling-mounted dynamic body-weight support and fall protection system that features highly specialized Patient Management Software that tracks performance by session and task. New to the portfolio is the SafeGait ACTIVE Dynamic Mobility Trainer, built as a cost-effective, non-robotic fall protection system that enables full dynamic movement, and the SafeGait EMBRACE Rehabilitation Harness, all designed in collaboration with therapists.
ProtoKinetics, Havertown, Pa, reports that the literature indicates more falls occur during transitional movements than during straight-line walking. In addition, postural control, dynamic balance, and transitional gait performance (starting, turning, braking) are critical components to quantify in clinical practice. That is why the company developed the PKMAS Primary Gait Screen (PGS). The PKMAS PGS addresses transitional movements in a single test. It is designed to be extremely easy to administer and offer immediate results that require no editing.
Solo-Step Inc, North Sioux City, SD, provides the Solo-Step Track System, which consists of a high-performance, overhead aluminum track and trolley mounted to the ceiling. An attached harness provides support for patients during all aspects of physical therapy, including sit-to-stand, gait training, and balance training. The system is engineered to allow these therapies to be performed with one therapist, reducing staff time and workers’ compensation claims.
In-Step Mobility Products Inc, Skokie, Ill, is a manufacturer of advanced rolling walkers for walking rehabilitation and neurological conditions. Updated for 2016, the company offers the U-Step 2 Neurological Walker, designed to provide superior stability to prevent falls. The reversed braking system is operated with a single hand, and additional features include rolling resistance adjustment, laser and auditory cueing for gait training, and Parkinson’s freezing. Custom platforms are available for this device, which reportedly is Medicare reimbursable.
– Frank Long[/sidebar]
Advances in Pediatric Mobility
Our ability to make progress with pediatric SCI patients is tied directly to an increased understanding of the ability of the human body. Significant advances have been made in the understanding of how the brain and spinal cord are wired and their capacity to rewire after injury or disease. It was previously believed that the role of the spinal cord in locomotion was much like a telephone cable that simply relayed signals to walk or step from the brain to lower-extremity muscles. Thanks to basic science, it is now known that the spinal cord is not just a telephone cable but actually is, to some degree, “smart.”
As it develops, the central nervous system (CNS) brain is highly dependent on and is modified and shaped by sensory experience. The brain and spinal cord can adapt their structural organization to new situations resulting from developmental and environmental situations, such as an injury—this is called “neuroplasticity.” Studies have shown that even after a severe injury, if provided with an intense repetitive pattern of sensory information, such as the motions of stepping or walking, the spinal cord can, over time, rewire itself as well as use intact pathways and eventually generate a motor response. This knowledge has given rise to new rehabilitation strategies and techniques, such as electrical stimulation, and activity-based therapies have emerged, including locomotor training (LT).
Locomotor Training Principles and Practice
LT is an intensive activity-based therapy that uses intense repetitive practice to activate the neuromuscular system below the lesion to complete a specific task (eg, sitting, standing, or walking). It works to “awaken” dormant neural pathways by repetitively stimulating the muscles and nerves in the lower body, trunk, or arms—allowing patients with SCIs to regain motor abilities and function.
LT is still relatively new and not yet widely available. However, some rehab facilities are beginning to offer various versions of it, including Frazier Rehab Institute, in Louisville, Ky, a part of KentuckyOne Health. As part of the Christopher & Dana Reeve Foundation NeuroRecovery Network (NRN)—a cooperative network of rehab centers across the country—I’m closely involved with nationwide efforts to deliver LT in a standardized evidence-based, three-part protocol:
- Step Retraining Using Partial Body Weight Support on a Treadmill (BWST) and Manual Facilitation
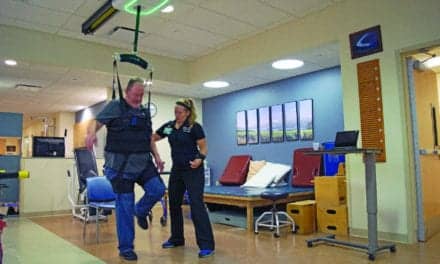
In LT sessions, the patient affected by paralysis or paresis is suspended over a treadmill in a specialized harness that supports a portion of their body weight. Specially trained therapists manually facilitate the patient’s limbs, pelvis, and trunk to simulate walking and standing, thus providing the spinal cord with an appropriate sensory pattern consistent with the activity.
- Over-Ground Assessment
As the patient’s skills and function improve in the treadmill environment, the therapists assess the transfer of skills off the treadmill with manual support and/or assistive mobility equipment. Depending upon the advances made, the emphasis may include stepping over-ground, improving trunk control and balance during sitting, standing, and stepping; and/or improved standing. This aspect sets the stage for recommendations for the patient (parent/family) as to choices made for daily incorporation of training principles and skills into daily life, ie community integration.
- Community Integration
The training principles used in step retraining and the skills acquired by the patient are then transferred to daily life activities at home, school, and in the child’s community. This extends training beyond the clinic and effectively increases the training time and benefit for the patient. LT consists of a continuum of training principles that are applied across the three training environments.
This is the protocol used in the pediatric rehab program at the Frazier Rehab Institute in Louisville, Ky. The program features an outpatient pediatric LT clinic that sees about eight patients per day who are affected by various mobility disorders, many of whom travel great distances for treatment.
Locomotor Training Process in Pediatric Patients
Children are sometimes referred to as “busy bodies” for good reason. Activity is the hallmark of childhood. Children want to roll, run, sit up, kick a ball, and play. When these abilities are taken away due to a spinal cord injury, a cascade of effects is seen, paralysis being the most obvious. In pediatric SCI patients, a child’s developing anatomy and life experiences greatly impact injury patterns and subsequent care. This physical and psychological maturation, along with common secondary complications associated with SCIs, requires a treatment plan unique to each child (and family) in concert within the paradigm of activity-based therapies.
At Frazier Rehab Institute, children as young as age 1 year through age 18 years are treated. Patients undergo a thorough assessment to determine eligibility for LT. Once enrolled, they participate in 1.5-hour LT sessions 5 days a week for a minimum of 60 sessions in a specialized gym. Activity-based therapies are most successful when the principles are incorporated throughout the child’s day at home, school, and in community settings, so the role of family is vital, and the program offers parents or caregivers active roles throughout the treatment. Children who have suffered a severe SCI require intense, repetitive training to see results. Children must have ample opportunities to practice skills they’ve gained during the day, which can be as simple as placing the child outside of a wheelchair to a place on the floor, allowing use of new mobility, or into a rocking chair to encourage use of trunk muscles.
[sidebar float=”right” width=”250″]Product Resources
The following companies also provide products for gait and balance:
APDM
Aretech
Biodex
Bioness
Clarke Health Care Products
GAITRite/CIR Systems Inc
Gorbel Medical/SafeGait
In-Step Mobility Products
Mobility Research
Motorika Medical Ltd
ProtoKinetics
Saebo Inc
Solo-Step
Tekscan
Vista Medical
www.boditrak.com[/sidebar]
Locomotor Training Equipment
Technology plays a central role in LT, and therapists rely on an arsenal of tools to maximize LT. Currently, BWST systems are the most commonly used, though technologies such as robotic LT systems have joined the market in recent years. While the advent of specialized equipment is exciting, it is important to note that clinicians must not equate novelty with efficacy. When considering LT equipment, the emphasis must be on the goal and the scientific foundations of the therapy.
Equipment used in Frazier Rehab Institute’s NeuroRecovery Network adult LT program includes the PowerNeuroRecovery closed-loop computer-controlled BWS system that allows center of mass movement while controlling a constant body weight support. The device allows control of treadmill speeds from 0 to 10 mph, and has seating and foot-support systems that include ergonomically appropriate support design for staff safety. The BWS system is supplemented by various other tools that each provide unique modes for physical performance testing or for delivery of a goal-directed therapy. These include:
- A GAITRite computerized pressure-sensitive gait mat/walkway that records footfall pattern and provides spatial-temporal parameters of gait. Walking speed is one of the measures overall ambulatory function. This tool from GAITRite/CIR Systems Inc, Sparta, NJ, allows therapists to measure gait in a simple automated way without any encumbering attachments.
- Harnesses of various sizes. The attributes of the harness are important for patient safety, therapist and trainer protection from injury, and optimal step training. Correct harness fit is essential and should be established on the first day of training to maximize comfort and expedite preparation for future training sessions. Improper harness fit can affect the quality of the stepping by putting the client at a kinematic disadvantage by causing trunk flexion or hyperextension, excess trunk lateral movement, and hip extension limitation.
- Additional tools include mirrors that provide visual feedback, a variety of assistive devices, automatic blood pressure monitoring equipment, a portable step counter, and supplies that include a stop watch, yardstick, curbs, reclining chair, and an automatic blood pressure, heart rate, and oxygen saturation monitor.
Key Considerations for BWST Systems
- Patient safety and trainer ergonomics are important considerations when choosing a BWST system. The system should allow for comfortable trainer positioning with easy access to the patient’s hips and legs. Also, seat adjustability for optimal trainer positioning enhances the effectiveness of the training and long-term health of the trainer.
- A feedback system indicating the immediate load during all standing or stepping activities on the treadmill is optimal because it provides online information for establishing training goals and monitoring the client’s response. A dynamic
feedback system that constantly adjusts the BWS to maintain support and allows the typical sinusoidal pattern of the body’s center of mass during walking optimizes the retraining of the nervous system for over-ground walking. - A proper BWS system must have a safety mechanism that
prevents falls but also provides enough leeway for the patient to stumble, trip, or misstep during walking, and allows them to self-correct their step and balance to prevent a fall. Additionally, the system must include a provision for releasing the client from the support quickly, if needed. - BWS systems for adults: Several companies offer BWS systems to the PT market that are feature-rich and designed for use with adult patients. Aretech, based in Ashburn, Va, offers the ZeroG Gait and Balance Training System and ZeroG Lite. The SafeGait 360° Balance and Mobility Trainer is available from Gorbel Medical, Fishers, NY, while Valencia, Calif-based Bioness provides the Vector Gait & Safety System. North Sioux City, SD-headquartered Solo-Step Inc is also a provider of BWS technology, and offers two versions of its Solo-Step Overhead Track & Harness Systems to the therapy market.
When it comes to equipment for children, one of the key factors to consider is their size. Having children use adult equipment is akin to expecting a 20-pound child to ride an adult bicycle, which does not make practical sense. Pediatric LT equipment must be proportional to not only the child, but also the clinicians and trainers guiding the therapy.
Advantages of a BWST Systems in Locomotor Training:
- Patients can be aligned into an upright posture and incrementally increase the load-bearing capacity of their lower extremities.
- The harness ensures that patients won’t fall, which helps boost their confidence and allows them to focus fully on the task at hand.
- The treadmill helps drive the patient’s legs and provides an adequate speed of walking, which is often unattainable by their own control.
While there are several BWST brands marketed for adults, no specialized options exist for the pediatric population that meet both the needs of children and the trainers. Our interdisciplinary team of engineers, scientists, clinicians, and industrial design specialist has received funding from the Coulter Translational Award Partnership Program at the University of Louisville, Speed School of Engineering to develop a training system specially designed for children. The first prototype will be tested this year at Frazier Rehab Institute, with the goal of making the treadmill commercially available to therapists as early as 2017. PTP
Andrea Behrman, PhD, PT, FAPTA, is a professor in the Department of Neurological Surgery, University of Louisville, Louisville, Ky. Her research focus is to develop and test therapeutic interventions promoting recovery after spinal cord injury in children and adults capitalizing on activity-dependent neuroplasticity and an understanding of the neurobiology of walking and motor control. Behrman leads the Outpatient Pediatric Locomotor Training program at Frazier Rehab Institute, part of KentuckyOne Health. For more information, contact [email protected].