Consistent physical therapy with tried-and-true techniques helps patients with neurological damage restore compromised functions.
By Deborah Struiksma, PT, NCS
Imagine experiencing a life-changing event such as a stroke, traumatic brain injury, or spinal cord injury that impacts your everyday quality of life. You just want to be “normal” again, but how do you get there? Oftentimes victims of neurological damage choose to wait things out hoping that their symptoms will eventually resolve on their own without accepting aid. But you know as well as I do that, unfortunately, that hope is not rooted in reality. To minimize losses after neurological injury, individuals must focus on promoting neuroplasticity to reorganize the central nervous system’s neural circuitry and restore compromised functions. Similarly, for individuals with chronic neurological conditions, physical therapy can help keep their symptoms from worsening.
Why? In both instances, it’s that age-old adage “use it, or lose it.” Put simply, in order to gain or retain proficiency over a function you must practice it regularly. The good news is that we as physical therapists can use tried-and-true products and techniques to provide hope for many through consistent physical therapy-based rehabilitation.
Components of a Successful Physical Therapy Program for Neurological Damage
The truth is that there actually is no such thing as a typical long-term physical therapy program because every recovery path is based on an individual’s unique conditions and personal interests. In motor learning, clients need meaningful tasks in order to make the exercise more effective and create a greater lasting effect on the central nervous system. Remember that if an activity resonates more with a patient, they often push themselves harder, and their attention shifts from their symptoms to the task itself. They will also likely remember the task more effectively.
For example, if someone who was an avid pickleball player and is experiencing some type of paralysis on one side of their body as a result of their stroke, you can give the patient a racquet and then instruct them to do some type of volley activity while standing. In doing so, the patient is being kept standing bearing weight in a safe manner while also participating in a meaningful task they enjoy.
Although you’ll customize every program to fit the client’s needs, there are a few key standard components:
Repetition—The more your client practices working with affected functions, the stronger the newly rewired functions become. With repetition also comes error, which is needed so that the body can learn to make adjustments.
Consistency—Being consistent with home exercises can be one of the most challenging aspects for individuals going through a physical therapy program. Patients may need your help with therapy set-up, or need a friendly reminder to engage in their home exercises to begin with.
Challenge—You can give patients a target and then over time challenge them to increase their speed and intensity. Doing so promotes adaptive changes and functional improvement.
For patients with neurological issues, goals center around the patient eventually being able to resume doing everyday tasks. These tasks can include, but are not limited to, standing again for the first time, bearing weight on a weaker side of the body, walking, and running everyday errands. Whatever the tasks and goals may be, it’s important to give patients home strengthening programs that include exercises that fall within their own personal limitations.
PRODUCT RESOURCE
The following companies provide technologies that can be useful in the treatment of stroke and neurological conditions:
Tools for Neuroplasticity
When working to improve neuroplasticity for those going through a neurologically based rehab program, it’s best to employ tools you can use to help facilitate motor activity while oftentimes also implementing cognitive components. Here are examples of products that I find helpful for these goals during physical therapy for neurological damage in my practice.
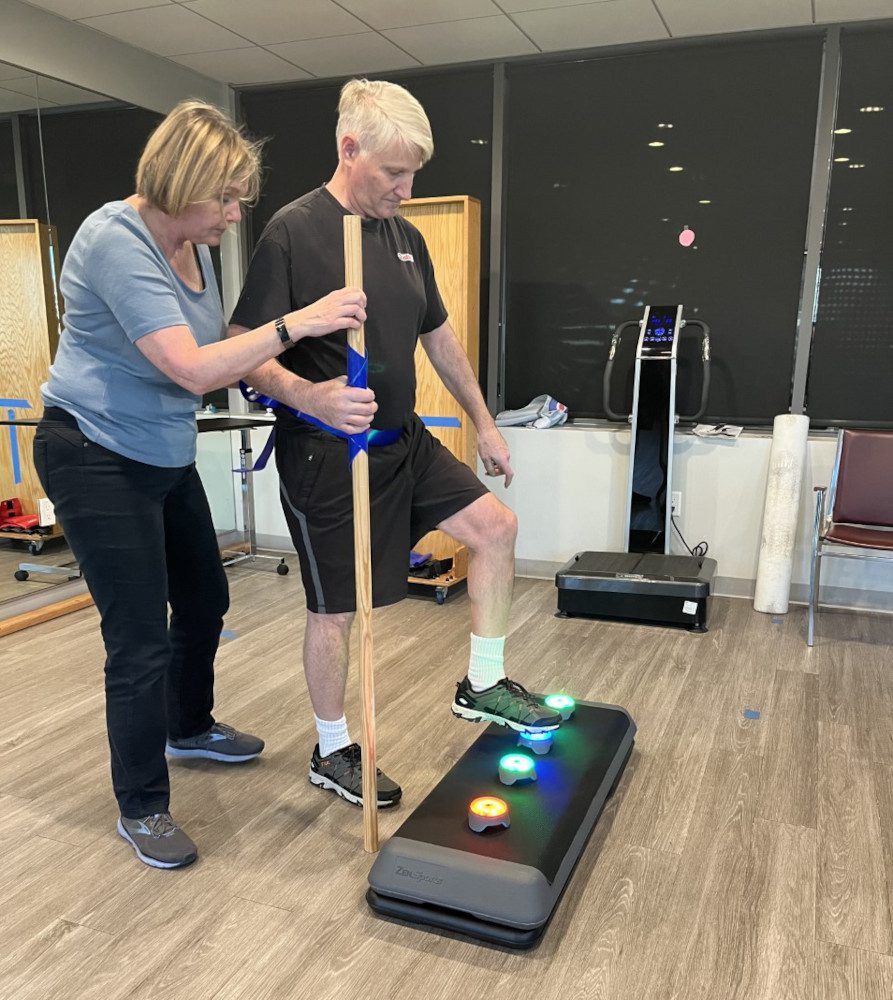
Reaction Training Lights
With reaction training lights, you can have patients participate in drills that challenge both their cognitive abilities through their reaction timing and their physical abilities. You can set up the colored light pods or screens through the use of an app. Patients will be asked to hit the lights to turn them off or may be asked to target a particular color of light to interact with. The lights can be adjusted to work in different intervals, speeding up or slowing down the pace at which they light up. These types of lights include BlazePods from BlazePod, Tel Aviv, Israel; the FitLight System from FitLights, Ontario, Canada; Reflexion from Reflexion Interactive Technologies Inc, Lancaster, Pa; and Reax Lights Pro from Reaxing North America LLC, Simi Valley, Calif.
There are many ways you can integrate these reaction training lights into physical therapy sessions. You can challenge patients to see how many “hits” they can get by touching the light in a designated amount of time, or ask them to move in a side-stepping motion to stomp on a light pod to turn it off. You can use these training lights to create a cognitive component by having the patient figure out which color to hit, and you can incorporate a speed component by asking a patient to get a pre-determined number of hits on the lights within a designated number of seconds.
Bodyweight Sling Support System
Patients are slipped into a sling or harness that unweights, protects, and moves with the patient as they practice average daily living activities one-on-one with their therapist. They are particularly useful when accompanied by a treadmill in getting patients to regain their walking pattern. Companies that produce these support systems include Minneapolis-based DIH Technology; Shirley, NY-based Biodex; Mobility Research Inc, Tempe, Ariz, with its LiteGait; and Aretech LLC, Sterling, Va, which offers the ZeroG Gait and Balance System.
Functional Electrical Stimulation
Normally when a part of the body needs to move, the brain sends electrical signals through the nervous system telling muscles to react. In individuals with neurological damage, these signals don’t work as well as they should. When using Functional Electrical Stimulation (FES) as a treatment, an electrical current is applied externally over a nerve or over the bulk of a muscle to help the muscle contract. While using FES, I ask patients to complete reaching-based tasks by grabbing larger items such as cups or even small cones. As their grip improves, I slowly scale down the size of the objects until they are successfully able to pick up very small items such as coins.
Hand Therapy Rehabilitation Gloves
There are four different types of hand therapy gloves: static hand braces, edema gloves, assistive gloves, and hand therapy exercise gloves, such as those available from Flint Rehab, Irvine, Calif. Each type serves a different purpose, but one particular variety provides stimulation, thereby helping to drive motor activity and help with spasticity.
Boxing Gloves
Noncontact boxing’s varied and high-intensity workouts offer a blend of strength training and cardiovascular conditioning. When used for physical therapy, simply adapt exercises from the boxing realm that emphasize agility, speed, endurance, accuracy, hand-eye coordination, footwork, and strength. The reaction timing element of boxing also incorporates cognition. The long-term intention is that these exercises will eventually improve agility, coordination, and balance.
Hand Grips, Straps, and Walkers
Hand grips placed on walkers with a patient’s hand safely strapped on the walker can promote the hand to become weight-bearing, thereby providing the neurological system with bilateral feedback and helping to create symmetrical movement on both sides. This can be particularly helpful for stroke victims who are experiencing difficulties with their shoulder complex or areas down through their arm.
Setting Patients Up for Success
Coping with neurological function loss is challenging, but effective physical therapy for neurological damage can help set patients up for success. Approximately 70% of stroke survivors encounter upper limb and/or hand weakness as a result of their stroke. If neglected, conditions such as spasticity can set in. Furthermore, recent studies have shown that physical therapy may help improve or stabilize symptoms of Parkinson’s Disease. For those with spinal cord injuries, regular cardiovascular training has often resulted in improved independence in daily activities because regular training improved cardiovascular function, aerobic capacity, and exercise tolerance. The latter are just a few examples, but the list does go on. With the right recovery plan and tools, you can put patients on a positive path toward a better quality of life.
Deborah Struiksma, PT, NCS, is a physical therapist at Complete Balance Solutions, an outpatient neurologic rehab institute in Seal Beach, Calif. Her specialty area of practice is vestibular rehabilitation and she is dedicated to the treatment of individuals with dizziness, imbalance, and neurologic disorders. She received her Neurologic Clinical Specialty Certification in 2005 and Re-Certification in 2015. For more information, contact [email protected].





