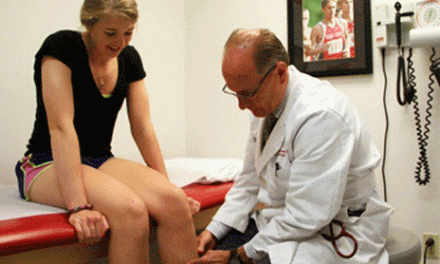
Depicted is the start position of the Dix-Hallpike test for Benign Paroxysmal Positional Vertigo (BPPV).
By Kelsi Smith, PT, DPT
Vertigo by definition is an abnormal sensation or perception of motion or spinning. Individuals with vestibular dysfunction often report symptoms of vertigo, dizziness, imbalance, and/or visual disturbances. Approximately one third of all reported healthcare visits include symptoms of dizziness and vertigo.1 It is the second most common complaint heard in doctor’s offices, and will occur in 70% of the nation’s population at some time in their lives.1
Vestibular dysfunction often leads to increased risk for falls. In 2013, the direct medical cost of falls, adjusted for inflation, were $34 billion, 2 and by the year 2020 the annual indirect and direct costs of fall-related injuries is predicted to reach $54.9 billion.3 Eighty percent of people 65 years and older have experienced dizziness of some kind, with Benign Paroxysmal Positional Vertigo (BPPV) being the most common, affecting around 50%.1 Vestibular rehabilitation for the treatment or management of patients with vestibular dysfunction has increased as the knowledge base continues to grow and develop.4
Brief Review of Background of Vestibular Conditions
The vestibular system is comprised of three compartments which relay information to the brain about how the head is moving in relation to the world. Dysfunctions can occur in any of the sections of the ear (outer, middle, inner) and can cause unilateral vestibular hypofunction (BPPV, Meniere’s Disease, labyrinthitis, vestibular neuronitis, acoustic neuroma, Perilymphatic Fistula [PLF]), or bilateral vestibular hypofunction (ototoxicity, bilateral hearing loss, PLF).
[sidebar float=”right” width=”250″]Product Resources
The following companies provide equipment for vestibular rehabilitation:
AMTI
www.amti.biz
APDM Wearable Technologies Inc
www.apdm.com
Aretech LLC
www.aretechllc.com
Biodex Medical Systems
www.biodex.com
Body Craft
www.bodycraft.com
CSMi
www.csmisolutions.com
GAITRite – CIR Systems Inc
www.gaitrite.com
GNR Rehabilitation & Fitness Products
www.gnrcatalog.com
Gorbel Medical
www.safegait.com
Hocoma
www.hocoma.com
Hoggan Scientific LLC
www.hogganhealth.net
In-Step Mobility Products Inc
www.ustep.com
Landice
www.landice.com
M.A.S.S Rehab Inc
www.rehabharness.com
Med-Fit Systems
www.medfitsystems.com
Micromedical Technologies Inc
www.micromedical.com
Mobility Research Inc
www.litegait.com
Natus Medical Inc (NeuroCom)
www.onbalance.com
novel electronics
www.novelusa.com
Perry Dynamics Inc
www.perrydynamics.com
ProtoKinetics
www.protokinetics.com
Solo-Step Inc
www.solostep.com
Tekscan Inc
www.tekscan.com[/sidebar]
First-Time Experience of Vertigo
Many individuals who attend an initial evaluation for vestibular rehabilitation are frustrated, anxious, fearful, and/or confused about their symptoms. Common description of symptoms include: “I feel dizzy,” “I felt like my whole world was spinning,” “I don’t feel steady,” “I need to hold onto something or I will fall over,” or “I feel like I am in a cloud/feel foggy.”
One article describes vertigo as “primal terror,” the emotional experience with one’s inability to naturally maintain one’s balance in opposition to gravity and to integrate vestibular input.5 As a clinician, it is imperative to take a thorough history and ask follow-up questions that will lead to correct identification of associated symptoms, especially differentiating between dizziness, vertigo, and imbalance.
Common symptom complaints can vary between vestibular diagnoses, as follows:
BPPV
• Vertigo, frequently described as the “room spinning” with changes in head position relative to gravity (eg, getting in and out of bed, rolling over in bed, bending forward, or looking up)
• Symptoms last seconds
Meniere’s Disease
• Fullness/pressure in one ear, balance problems, light-headedness, headache, hearing loss, roaring tinnitus
• During the time of an attack, individuals may report severe or sudden vertigo that is debilitating
• Symptoms last hours to days
Acoustic neuroma
• Hearing loss in one ear, or constant ring/buzz in one ear
• Feels as though balance is off/need to hold onto someone or something
• Numbness/tingling on one side of the face/headaches
Labrynthitis
• Recent cold/viral infection and started feeling dizzy/vertigo; acute phase-constant vertigo
• Acute hearing loss or tinnitus
• Sensitive to quick head turns and/or symptoms provoked with more than one position
Vestibular neuronitis
• Same as labrynthitis; however, patients do not report any hearing loss or ringing
Cardiovascular (orthostatic hypotension)
• Symptoms increase with sitting up or standing up quickly
• Feels faint and light-headed, but no room spinning
Brain Injury/Post-concussive syndrome
• Dizziness, nausea, and constant vertigo
• Anxiety about symptoms or delaying return to sport/activity
• Symptoms increase with exertion
Perilymphatic Fistula (PLF)
• Fullness/pressure in one ear, hearing loss that comes and goes, but no true vertigo, sensitivity to motion
• Symptoms increase with riding an elevator, traveling on a plane, going over a mountain
Persistent Perceptual and Postural Dizziness (3PD) formerly known as Chronic Subjective Dizziness (CSD)
• Persistent sense of dizziness/unsteadiness, feeling constant motion (rocking or swaying)
• Increased with standing, walking, sitting
• Intolerant to complex environments
• May be preceded by a true physiologic history of vestibular dysfunction
A distinct overlap in subjective complaints reinforces the importance of a thorough interview/history.

This individual is undergoing a vestibular
habituation activity to address visual scanning and tracking as she is asked to search for certain numbers called out by the clinician. The treadmill provides a sustained ambulation speed while the individual carries out a secondary task.
Vertigo’s Debilitating Impact
Vestibular dysfunctions are debilitating and can be the cause of reliance on social support, absenteeism, and increased healthcare burden. A 2008 study, “Burden of Dizziness and Vertigo in the Community,” found a statistically significant difference between non-vestibular dizziness and vestibular vertigo.6 The healthcare burden (medical consultation requests) increased to 70% from 54%.6 Many patients report missing work, decreasing work duties, or report decreased activity levels as a result of their symptoms. In particular, vestibular vertigo accounted for 41% claiming sick leave, 40% interruption of daily activities, and 19% avoidance of leaving the house.6
Based upon these statistics, it is important to use objective scales to assess for baseline symptoms and determine current level of function (ie, Dizziness Handicap Inventory, Motion Sensitivity Quotient/Test, Vertigo Symptom Scale [0-10], Activities-specific Balance Confidence [ABC] scale, or Neck Disability Index [NDI]). These scales can also help the clinician reveal important subjective symptoms that the individual may not be able to narrate or verbalize.
Additionally, it is useful to include an objective balance measure to assess for fall risk (ie, Dynamic Gait Index [DGI], Clinical Test of Sensory Integration of Balance [CTSIB], Berg Balance Scale [BBS]). According to the National Institute on Deafness and Other Communication Disorders (NIDCD), 4% (8 million) of American adults report a chronic problem with balance,1 and falls account for 10% of hospitalizations and for 50% of accidental deaths among the elderly.3
Education is Key During Initial Evaluation
As a clinician working with vestibular dysfunction, patient education is essential. Patients have the tendency to use the catch-all term, “dizziness.” Our first educational goal is deciphering symptoms of “vertigo” (ie, room spinning/world spinning) from dizziness (ie, light-headedness, cloudy, fuzzy, foggy). It is also important to determine if there is imbalance, nausea, or tinnitus. Once this information is obtained, the clinician can begin the differential diagnosis and determine cause of symptoms.
Many individuals do not receive information about their condition and find comfort in knowing statistics, prognosis, and understanding pathology. For those with BPPV, using analogies and multiple media forms to educate (ie, pictures, videos, models, demonstrations) can be very helpful. Particularly with this patient population, walking patients through the purpose behind specific examination items and how that information correlates to their symptoms is imperative. Education is vital to successful management of their condition.
What People Learn Online
As technology continues to grow, so too does the amount of information available on the Internet. Many patients begin to look their symptoms up and link their condition with a severe disease or diagnosis, as dizziness can be an initial sign of stroke. This can create anxiety in some patients and create a hyper-vigilant state when they attend initial evaluation. In addition, those who are told they have BPPV may try to find ways to correct it by themselves and attempt to complete a self Epley maneuver. However, they run the risk of complicating repositioning efforts of otoconia due to improper positioning and lack sufficient understanding of pathology.
[sidebar float=”right” width=”250″]Additional Harness & Balance Technologies
• A variety of body weight support technologies are available on the market to help bolster patient confidence, including the Bioness Vector Gait and Safety System15, available from Valencia, Calif-based Bioness; the ZeroG16 from Aretech LLC, Ashburn, Va; the ceiling-mounted Solo-Step System17 by Sioux Falls, SD-based Solo-Step; and the SafeGait 360° Balance and Mobility Trainer18 from Gorbel Medical, Fishers, NY, with Patient Management Software built to allow patient performance measures to be tracked and compared by task and session.
• Other manufacturers of balance technologies include Biodex Medical Systems Inc, Shirley, NY, which offers the Biodex Balance SD19 designed to improve balance, increase agility, and develop muscle tone. The Proprio Reactive Balance System,20 by Perry Dynamics headquartered in Decatur, Ill, is another balance system that can be used to challenge balance and reactions.[/sidebar]
Equipment Used for Vestibular Rehabilitation
In regards to treatment for vestibular dysfunction, a variety of equipment is available from a rehabilitation perspective.
A few are listed below:
- Chatham, Ill-based Micromedical Technologies Inc’s RealEyes7 for assessment of nystagmus resulting from changes in position of the head or head motions. For some, this may increase anxiety or cause feelings of claustrophobia.
- APDM mobility lab8 computerized posturography for modified Clinical Test of Sensory Integration of Balance (mCTSIB) and instrumented gait, available through APDM Wearable Technologies Inc, Portland, Ore. For many individuals with true vertigo or dizziness, these assessments are where individuals feel uncomfortable or insecure about their balance. From the clinician’s perspective, we are learning what system (visual, vestibular, somatosensory) the individual relies on and/or where there is a deficit.
- Adjustable tables with tilting headrest9,10 or wider mat platforms11, such as the Hausmann Upholstered Mat Platform by Hausmann Industries Inc in Northvale, NJ, allow for postural changes of the head into flexion and allow for height adjustment for body mechanics of the clinician as well as ability for support of lower extremities on the floor. This allows for increased patient comfort and ease. A variety of adjustable tables with tilting headrests are on the market, including the PT 250 and PT 350 tables, from Oakworks Medical Inc, New Freedom, Pa, as well as the 3 Section “Sierra” BAL 1060 table, offered by Stonehaven Medical Balance, Yorba Linda, Calif.
- The RehabHarness by M.A.S.S Rehab Inc in Englewood, Ohio, body weight support harness12 with Landice treadmill13 from Landice, Randolph, NJ, and NeuroCom SMART Balance Master by Natus Medical Inc, San Carlos, Calif14 allow the clinician to introduce a more complex and rehabilitative environment to address visual, somatosensory, and vestibular mismatch to begin reintegration of the balance system. The harness is built to provide a safe environment for an individual to practice, which is critical for building confidence.
When seeking an optimized outcome for patients, there are three keys to success:
1) Listening
2) Therapist education and confidence with accurate diagnosis
3) Effective patient education. For successful education, the clinician should take time to explain expectations toward resolution (despite perfect treatment) (ie, symptoms 10 to 24 hours post-treatment).
The prevalence of vertigo is high. Understanding the patient perspective will aid in patient rapport, improve patient care, and target specific intervention strategies. Individuals with these symptoms are highly motivated to recover. When paired with proper education, this motivation can greatly improve compliance in vestibular rehabilitation and expedite recovery. PTP
Kelsi Smith, PT, DPT, received her Doctorate in Physical Therapy from Washington University in St Louis in 2014. She is currently employed at Northwest Rehabilitation Associates in Salem, Ore. Her primary patient population includes multiple sclerosis (MS), Parkinson’s disease, stroke, vestibulopathy, healthy aging, and imbalance. Smith is also a lab assistant for second-year students at a local university and promotes health and wellness through exercise in the diabetic population. She does not endorse any specific product or company. Her clinical interests include use of aquatic therapy in MS, evidence-based management of vestibulopathy, and dual-task challenges in patients with neurological conditions. For more information, contact [email protected].
References
- Vestibular Disorders Association. http://www.vestibular.org. Updated 2015. Accessed May 1, 2015.
- Stevens JA, Corso PS, Finkelstein EA, Miller TR. The costs of fatal and non-fatal falls among older adults. Inj Prev. 2006;12:290-5.
- Dizziness and fall statistics and resources. Neuro Kinetics, Inc.: Experts In Balance. http://www.neuro-kinetics.com/landing_vestibular2.aspx. Accessed May 10, 2015.
- Hillier SL, McDonnell M. Vestibular rehabilitation for unilateral peripheral vestibular dysfunction. Cochrane Database Syst Rev. 2011;2:CD005397.
- Shaffer M. Primal terror: A perspective of vestibular dysfunction. J Learn Disabil. 1979;12:89-92.
- Neuhauser HK, Radtke A, von Brevern M, Lezius F, Feldmann M, Lempert T. Burden of dizziness and vertigo in the community. Arch Intern Med. 2008;168(19):2118-2124.
- Mobility lab. APDM Wearable Technologies Inc. Portland, OR. http://www.apdm.com/mobility/. Accessed April 2015.
- Video goggles: RealEyesTM. Micromedical Technologies Inc. Chatham, IL. http://www.micromedical.com/realeyes.html. Accessed April 2015.
- PT 250 and PT 350 tables. Oakworks Medical Inc. New Freedom, PA. https://www.oakworksmed.com/exam-treatment-tables.asp. Accessed June 11, 2015.
- 3 Section “Sierra” BAL 1060 table. Stonehaven Medical Balance, Yorba Linda, CA. http://stonehavenmedical.com/products.html. Accessed June 11, 2015.
- Hausmann Upholstered Mat Platform. Northvale, NJ. http://www.hausmann.com/product_pages/Matplatforms_mats_pillow.html. Accessed June 11, 2015.
- RehabHarnessTM. MASS Rehab Inc. Englewood, OH. http://rehabharness.com/product_list.php?listing=1. Accessed April 2015.
- T7 and T8 Rehab Treadmill. Landice. Randolph, NJ. http://www.landice.com/commercial-fitness/rehabilitation-physical-therapy. Accessed June 11, 2015.
- Balance and mobility: NeuroCom SMART balance master. Natus Medical Inc. San Carlos, CA. http://www.natus.com/index.cfm?page=products_1&crid=271&contentid=397. Updated 2015. Accessed May 30, 2015.
- Bioness Vector Gait and Safety System. Bioness Inc. Valenica, CA. http://www.bioness.com/United_Kingdom/Healthcare_Professionals/Vector_Gait_and_Safety_System.php. Accessed June 11, 2015.
- ZeroGTM. Aretech LLC. Ashburn, VA. http://www.aretechllc.com/overview.html. Accessed June 11, 2015.
- Ceiling mounted track system and harness. Solo-Step. Sioux Falls, SD. http://solostep.com/products/. Accessed June 11, 2015.
- SafeGait 360° Balance and Mobility Trainer. Gorbel Medical. Fishers, NY. http://safegait.com/safegait-system/. Accessed June 11, 2015.
- Biodex BalanceTM SD. Biodex Medical Systems. Shirley, NY. http://www.biodex.com/physical-medicine/products/balance/balance-system-sd. Accessed June 11, 2015.
- PROPRIO® Reactive Balance System. Perry Dynamics. Decatur, Ill. http://www.perrydynamics.com/Products/Default.aspx. Accessed June 11, 2015.
- Cost of falls among older individuals. Centers for Disease Control and Prevention. http://www.cdc.gov/HomeandRecreationalSafety/Falls/fallcost.html. Updated March 19, 2015. Accessed May 10, 2015.
- Agrawal Y, Carey JP, Della Santina CC, Schubert MC, Minor LB. Disorders of balance and vestibular function in US adults. Arch Intern Med. 2009;169(10):938-944.
- Balance disorders. NIH: National Institute of Deafness and Other Communication Disorders. http://www.nidcd.nih.gov/health/balance/balance_disorders.asp. Updated April 2014. Accessed May 10, 2015.
- Mansfield A, Wong JS, Bryce J, Knorr S, Patterson KK. Does perturbation-based balance training prevent falls? Systematic review and meta-analysis of preliminary randomized controlled Trials. Phys Ther. 2015;95:700-709.
- Neuhauser H, Leopold M, von Brevern M, Arnold G, Lempert T. The interrelations of migraine, vertigo, and migrainous vertigo. Neurology. 2001;56(4):436-41.
- Bisdorff A, Andree C, Vaillant M, Sandor PS. Headache-associated dizziness in a headache population: Prevalence and impact. Cephalalgia. 2010;30(7):815-20.
- Writer HS, Arora Rd. Vestibular rehabilitation: An overview. Int J Otorhinolaryngol Clin. 2012;4(1):54-69.
- Epidemiology of balance. Dizziness-and-Balance.com.http://dizziness-and-balance.com/disorders/dizzy_epi.html. Updated September 11, 2014. Accessed May 10, 2015.
Continuing Education Resources and Webinars
- www.healthclick.com/Live-continuing-education-courses.php
- www.vestibular.org/resources-professionals/build-your-practice
- http://learningcenter.apta.org/Courses.aspx